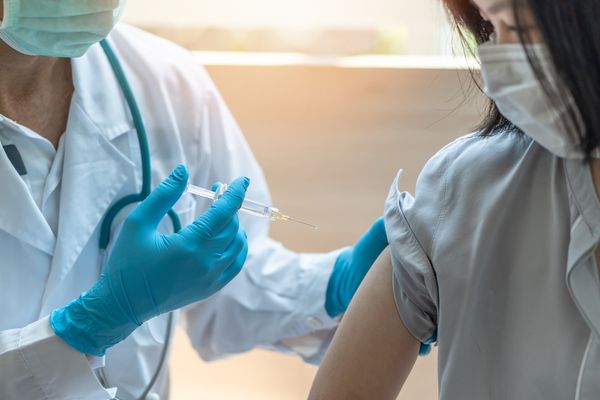
Across America, clinical trials, which are a vital step in bringing a new drug to market, have strikingly low rates of Black female participants. This is the case even with clinical trials centered on diseases that disproportionately affect African Americans in general or Black women in particular, such as including Alzheimer's, breast cancer, heart disease, stroke, diabetes and fibroids.
With more than 100 COVID-19 vaccine candidates currently in development around the world, it is essential that Black women be included in the COVID-19 clinical trials since the virus disproportionately affects African Americans.
Historically, clinical trials have largely included only white men, which means the findings on efficacy have been limited to that group. After 1993, progress was made to include more women in clinical trials, but severe race disparities remain — and that can skew results.
Unfortunately, the medical community has a long history of exploiting Black women in research, which has led to some distrust by the African American community. This distrust, along with the fact that the majority of trials are still designed by white men and exclude Black women, has led to the strikingly low rates of Black women's participation in medical research.
History of the exploitation of Black women in medicine
The lack of representation of Black women in modern clinical trials sharply contrasts with the high prevalence of Black women in exploitative medical experiments going back centuries. In fact, much of modern medicine was built on foundational discoveries that came at the expense of the health and livelihood of enslaved Africans.
Dr. James Marion Sims, often referred to as the Father of Modern Gynecology, carried out an extensive set of experiments on enslaved women throughout the 19th century without the use of anesthesia.
Black women and medical experimentation continued well into the 20th century. In 1951, a Black tobacco farmer, Henrietta Lacks, was treated for cervical cancer at Johns Hopkins Hospital. As detailed in "The Immortal Life of Henrietta Lacks" by Rebecca Skloot, unbeknownst to Lacks, her doctor took her cancer cells and they have been used in numerous experiments ever since — generating millions of dollars.
Two decades later, doctors experimented with the super coil abortion method on a small group of mostly young Black women. None of the doctors involved in the experiment had previous experience with the method, and the experiment left 60% of participants with complications and 20% with serious complications — twice the rate of saline abortions.
White men as the default
In spite of Black women and other minority groups having long been exploited for medical research, clinical trials have historically included only white men of European heritage.
"Medicine has traditionally been based on looking at the anatomy, physiology and biology of white men," explained Glenn Ellis, a medical ethicist.
It wasn't until 1993 that Congress passed the National Institutes of Health (NIH) Revitalization Act, calling for more women and minorities in clinical trials it supports, but the ruling only applies to federally funded research. And we're seeing the effects.
For example, in spite of the fact that African Americans are twice as likely to have Alzheimer's disease as whites, the clinical trials remain predominantly white, even if they include women or are all women. Notably, in one 2017 clinical trial for an Alzheimer's drug, only 1.6% of the trial participants were Black; 83% were white.
"The thing I worry the most about is that with [participation] rates of 3% to 5% for industry-sponsored trials and slightly higher for NIH-sponsored trials, there is a possibility, if not a great likelihood, that those medications may not work exactly as they do on white, European men," said Stephanie Monroe, the executive director of AfricanAmericansAgainstAlzheimer's at UsAgainstAlzheimer's.
In another example, a 2020 study analyzed one million patients with cancer in the United States and found that African Americans have a 28% higher cancer-specific mortality rate compared with whites. Nevertheless, Black patients represented less than 4% of all patients in multiple trials for treatments of lung cancer.
Lack of diversity begets lack of diversity
Two major factors in the disproportionate participation of Black women in modern clinical trials are the lack of diversity among researchers and the failure to simply ask Black women to participate.
"I can — on one hand — give you the leading African American principal investigator researchers in Alzheimer's disease," Monroe said. "I could maybe identify 10 in the whole country."
This illustrates a huge part of the problem. As Dr. John B. Sampson, associate professor at Johns Hopkins University School of Medicine, says, diversity in researchers can often lead to more diversity in participants.
"You cannot address the question of Black women in clinical trials without looking at the clinical trials themselves and seeing what the researchers are doing to recruit Black women," Sampson said.
Unfortunately, Black women are largely not being recruited for or even made aware of clinical trials. A 2017 Research America poll found that only 24% of African Americans stated that their doctor or other healthcare practitioner had ever spoken to them about medical research.
Monroe is doing what she can to change that, and when she presents statistics on Alzheimer's in communities of color, she asks if people would be interested in participating in clinical research. In general, the interest is there.
"They say, 'Yes, we would be really interested in learning what we qualify for.' We ask them, 'Have you ever been asked before,' and 85% say no," Monroe said.
How to increase the participation of Black women
Dr. Charlotte Owens is an OB-GYN and medical director of AbbVie who has completed successful clinical trials on uterine fibroids with a high representation of Black women.
"You have to take time to understand who you are trying to reach and their trusted sources of information. What do they read, listen to and watch? [It's important to be] omnipresent in all the places that the population you want to reach, trusts."
Another important way to improve Black women's participation is to make sure that women are completely informed about the nature of the trial in a way that is accessible to them. Languages and images used in marketing should resonate with women, and trials should be in locations close to their communities.
"Education and equal partnerships are critical to recruit patients to trials and to maintain their participation throughout the trials," Owens said.
She added that educating the families and loved ones of participants is another essential step to ensure that everyone is on the same page about what is happening so they feel like they're included and have a voice.
History can not repeat itself. The medical community needs to commit to creating diverse, equitable and accessible trials that welcome Black women as participants in innovative and potentially life-changing research.
Photo of Henrietta Lacks, Courtesy of the Lacks Family
- Why Do Women of Color Have Worse Breast Cancer Outcomes? - HealthyWomen ›
- Why Diversity in Clinical Trials Is Important - HealthyWomen ›
- Diversity in Cancer Clinical Trials - HealthyWomen ›
- Diversidad en los ensayos clínicos de cáncer - HealthyWomen ›
- Immunocompromised People and Covid-19 Clinical Trials - HealthyWomen ›
- Personas inmunodeficientes y ensayos clínicos del covid-19 - HealthyWomen ›
- Did You Know That Heart Disease Affects Women of Color Differently? - HealthyWomen ›
- COVID-19 and Diverse Participation in Clinical Trials - HealthyWomen ›
- HW Is a Convener on the COVID-19 Vaccine Education Project - HealthyWomen ›
- Congressional Briefing: Women in Clinical Trials - HealthyWomen ›