Like many reality TV stars before her, 2015 Big Brother contestant Meg Maley was keeping a secret. When viewers wondered why a seemingly healthy young woman did so poorly during physical competitions and was sometimes seen taking pills, Maley kept silent. It wasn't until after her season of the show ended that Maley revealed her secret: She had psoriasis and psoriatic arthritis (PsA).
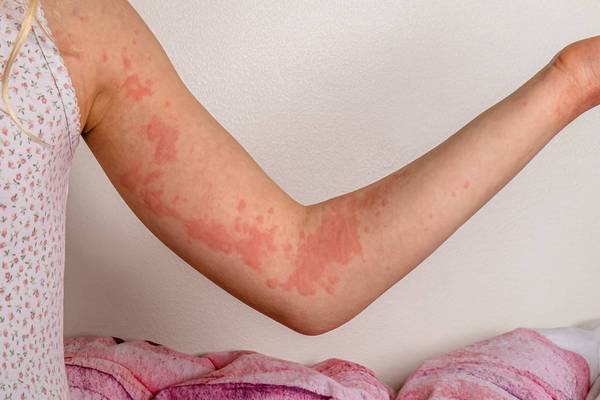
While many people think of psoriasis as a skin condition, it's actually a chronic autoimmune disease that can lead to serious health problems. Autoimmune diseases cause the body's immune system to mistakenly attack its own tissues and organs, which can lead to inflammation throughout the body.
This inflammation affects not just the skin but other tissues, organs and joints, and it can cause PsA, which is a form of arthritis that is characterized by joint swelling, stiffness and pain.
The effects of psoriasis can extend far beyond the skin. Having the disease also increases your risk of having obesity, diabetes, cardiovascular disease, mental health conditions like depression, and other autoimmune diseases, such as inflammatory bowel disease (IBD).
Being aware of the relationship between psoriasis, PsA and other health problems can help you recognize symptoms of these conditions — or prevent them from happening in the first place.
Signs and symptoms of PsA
Maley's PsA diagnosis is far from unusual for someone with psoriasis. PsA affects one in three people with psoriasis, can develop suddenly or progress slowly and can range from mild to severe. Symptoms of PsA include:
- Pain, stiffness and swelling in one or more joints
- Limited range of motion
- Soreness and stiffness in the morning
- Fatigue
- Swollen fingers and toes
- Eye irritation/inflammation (uveitis)
- Tendon or ligament pain
- Fingernail changes like pits (dents), horizontal lines or discoloration
Diagnosis and treatment of PsA
PsA can be hard to diagnose. "There's no specific blood test for it, as opposed to rheumatoid arthritis (RA) where many patients will have a specific antibody," said Dr. Stuart D. Kaplan, chief of rheumatology at Mount Sinai South Nassau in Oceanside, New York. Since the symptoms of PsA are similar to other immune-related diseases like RA, people with psoriasis may not know that what they think of as a skin problem can also affect their joints.
Your healthcare provider (HCP) or a rheumatologist (joint specialist) may use a physical exam, X-ray or blood test to diagnose PsA. They'll also want to know your medical history, including whether anyone in your family has psoriasis, PsA or other autoimmune disorders. About 40% of people with psoriasis or PsA have a family history of these diseases.
The sooner PsA is recognized, the easier it is to treat and manage. Early diagnosis of PsA can keep the disease from progressing, potentially preventing irreversible joint damage and permanent disability. "Psoriatic arthritis, like any inflammatory arthritis, destroys the joints," Kaplan said. "It causes what are called erosions in the bones, and once that happens, you can't undo it."
While there are always new and improved treatments on the horizon, some of the current treatment options for PsA are:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) — prescription or over-the-counter medications that can reduce inflammation and pain
- Corticosteroids — prescription anti-inflammatory medications
- Biologics, biosimilars and other disease-modifying antirheumatic drugs (DMARDs) — medications that can reduce inflammation and prevent PsA from progressing
PsA increases risk of other health problems
People with PsA may be more likely to develop certain health problems, some of them serious. A 2017 study found that patients with PsA have a 43% higher risk of developing diabetes compared to the general population and that there is a link between severity of PsA and diabetes risk. This means that the worse a person's PsA is, the greater their chance of developing diabetes.
PsA is also linked to health problems that often occur with diabetes, like obesity, high blood pressure and cardiovascular disease. Kaplan says the connection between obesity and PsA isn't well understood but that it may be related to the joint problems some people with obesity already have from carrying excess weight.
Obesity may also be a risk factor for PsA because fatty tissue causes a constant state of low-grade inflammation in a person's body, which is already a problem for people with PsA. But it's not just that obesity can make PsA worse — people with PsA may also be more prone to obesity, possibly because their joint pain prevents them from being physically active.
When it comes to cardiovascular problems such as high blood pressure and heart disease, people with PsA are doubly at risk. First, PsA itself is a risk factor for cardiovascular disease because the inflammation it causes can damage blood vessels. Second, people with PsA are more likely to have other risk factors for cardiovascular disease (like diabetes and obesity).
This combination of factors adds up to serious risk of cardiovascular problems. One analysis that included nearly 33,000 patients with PsA found a 43% increased risk of cardiovascular diseases in patients with PsA compared with the general population.
Being proactive about PsA
If you have psoriasis, it's a good idea to talk to your HCP about PsA even if you haven't noticed any symptoms. An early diagnosis can help you manage your illness — and lower your risk of developing the other conditions, such as diabetes, obesity and cardiovascular disease, that can go along with it. If you've already been diagnosed with PsA, it's worth asking your provider about new or different treatment options available to you.
After Maley went public about her PsA, she became an advocate for others with the disease. She told Arthritis Today that people shouldn't be afraid to ask questions or seek out a provider who will take their concerns seriously.
"I remember one doctor telling me that there were no more medicines and I just had to live with it, and that was crazy to me."
This resource was created with support from Bristol Myers Squibb.
- My Psoriasis Led to My Empowerment - HealthyWomen ›
- Living with Psoriasis My Entire Life, I Knew I Could Develop Psoriatic Arthritis - HealthyWomen ›
- Get the Facts About Psoriatic Arthritis - HealthyWomen ›
- Listen to Healthcare Providers, but Trust Your Body and Yourself - HealthyWomen ›
- Clinically Speaking: Questions to Ask Your HCP About Psoriatic Arthritis - HealthyWomen ›