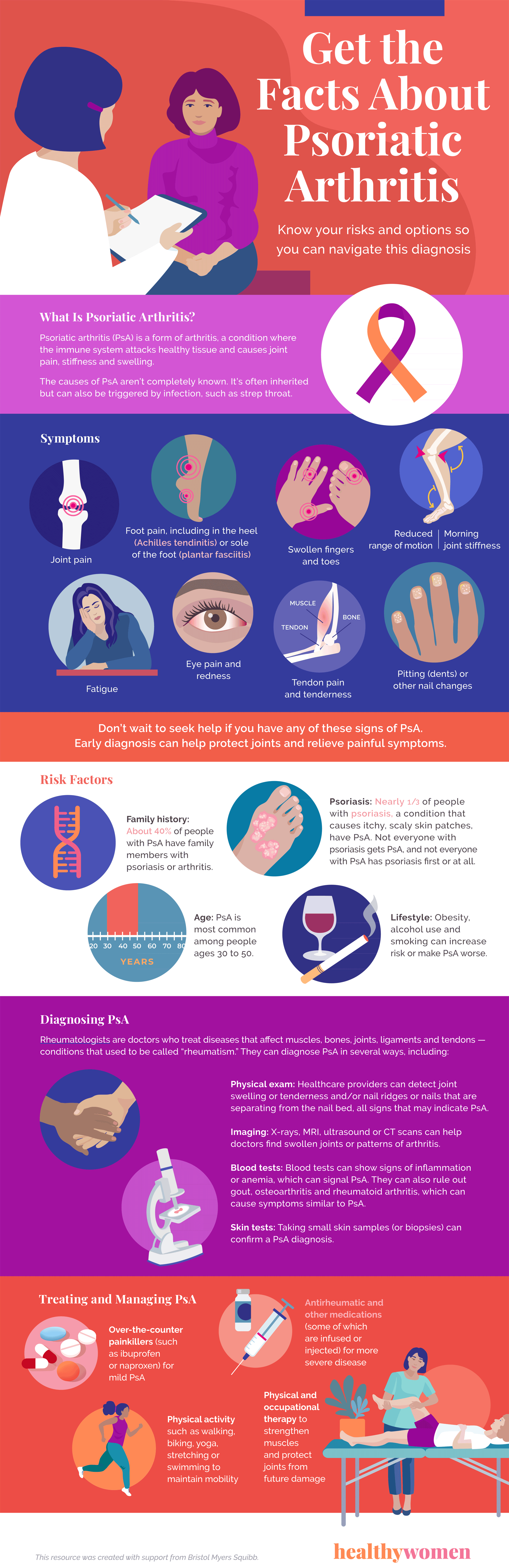
What Is Psoriatic Arthritis?
Psoriatic arthritis (PsA) is a form of arthritis, a condition where the immune system attacks healthy tissue and causes joint pain, stiffness and swelling.
The causes of PsA aren’t completely known. It’s often inherited but can also be triggered by infection, such as strep throat.
Symptoms
- Joint pain
- Swollen fingers and toes
- Foot pain, including in the heel (Achilles tendinitis) or sole of the foot (plantar fasciitis)
- Reduced range of motion
- Morning joint stiffness
- Fatigue
- Eye pain and redness
- Tendon pain and tenderness
- Pitting (dents) or other nail changes
Don’t wait to seek help if you have any of these signs of PsA. Early diagnosis can help protect joints and relieve painful symptoms.
Risk factors
- Family history: About 40% of people with PsA have family members with psoriasis or arthritis.
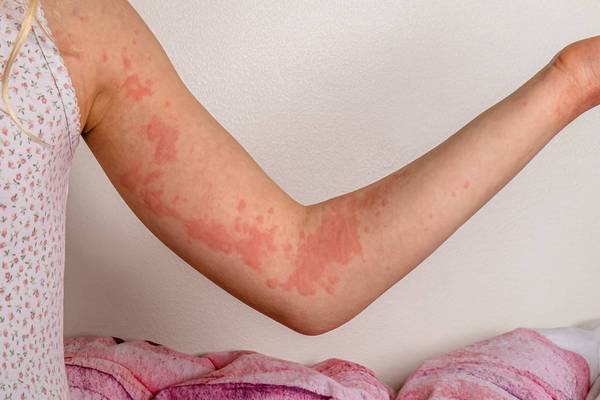
- Psoriasis: Nearly 1/3 of people with psoriasis, a condition that causes itchy, scaly skin patches, have PsA. Not everyone with psoriasis gets PsA, and not everyone with PsA has psoriasis first or at all.
- Age: PsA is most common among people ages 30 to 50.
- Lifestyle: Obesity, alcohol use and smoking can increase risks or make PsA worse.
Diagnosing PsA
Rheumatologists are doctors who treat diseases that affect muscles, bones, joints, ligaments and tendons — conditions that used to be called “rheumatism.” They can diagnose PsA in several ways, including:
- Physical exam — Healthcare providers can detect joint swelling or tenderness and/or nail ridges or nails that are separating from the nail bed, all signs that may indicate PsA.
- Imaging — X-rays, MRI, ultrasound or CT scans can help doctors find swollen joints or patterns of arthritis.
- Blood tests — Blood tests can show signs of inflammation or anemia, which can signal PsA. They can also rule out gout, osteoarthritis and rheumatoid arthritis, which can cause symptoms similar to PsA.
- Skin tests — Taking small skin samples (or biopsies) can confirm a PsA diagnosis.
Treating and managing PsA
- Over-the-counter painkillers (such as ibuprofen or naproxen) for mild PsA
- Antirheumatic and other medications (some of which are infused or injected) for more severe disease
- Physical activity such as walking, biking, yoga, stretching or swimming to maintain mobility
- Physical and occupational therapy to strengthen muscles and protect joints from future damage
This resource was created with support from Bristol Myers Squibb.
- 9 Common Misconceptions About Psoriasis - HealthyWomen ›
- My Psoriasis Led to My Empowerment - HealthyWomen ›
- Psoriatic Arthritis Can Put You at Risk for Other Health Problems ... ›
- Beyond the Physical: How Psoriatic Arthritis Can Affect Your Mental ... ›
- How Psoriasis Changes as Women Age - HealthyWomen ›
- Clinically Speaking: Questions to Ask Your HCP About Psoriatic Arthritis - HealthyWomen ›