One of the hottest topics in scientific research today is the microbiome and its effects on human health. Microbes appear to play a role in how we sleep, how likely we are to develop certain diseases and whether we’ll develop allergies — and seemingly everything in between.
What is the microbiome?
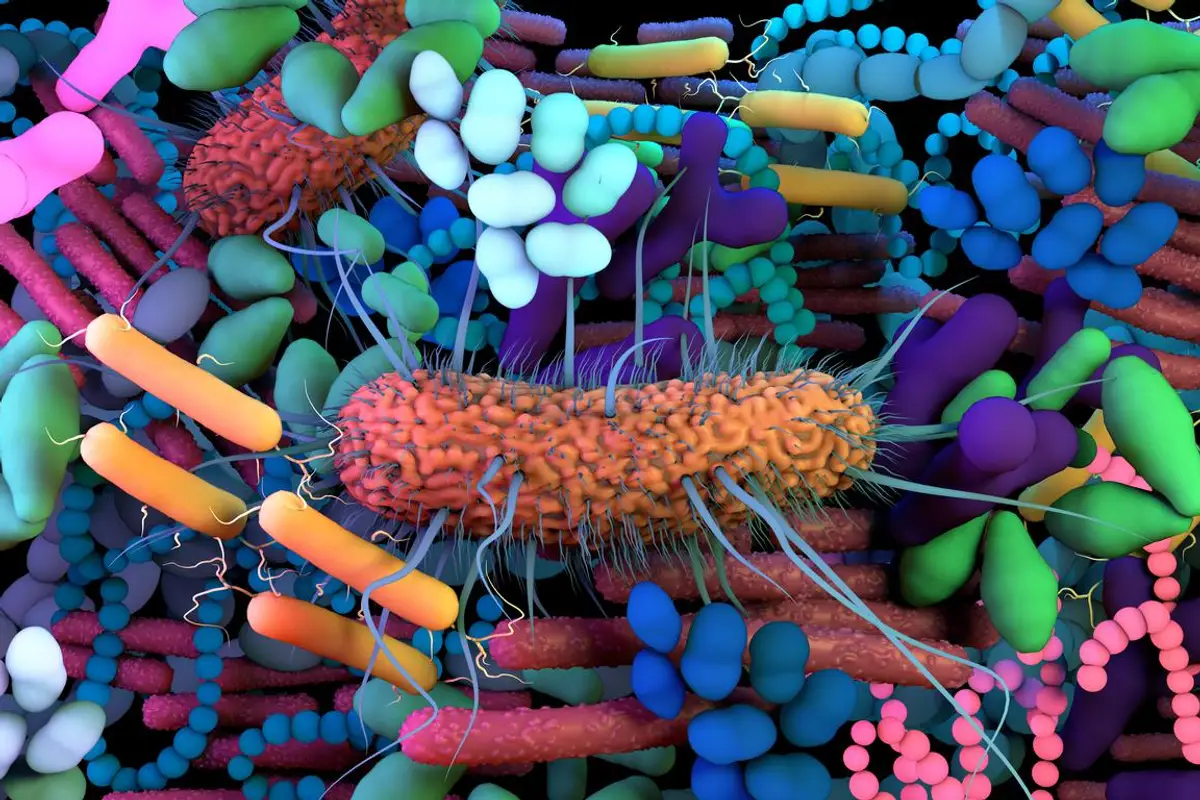
The microbiome is a group of microorganisms (also called microbiota or microbes) that live in a particular environment. These microbes include bacteria, viruses, parasites and fungi, which we sometimes just call “bugs.”
Each of us has our own, unique microbiome made up of trillions of microbes that respond to whatever we’re exposed to in our environment and whatever we put in our bodies, such as food and medicine.
“The microbiome is around 40 trillion cells comprising 200-500 different species of bacteria, and they produce a cornucopia of chemicals that our body has become reliant on over the last few million years of our evolution,” said Jack A. Gilbert, Ph.D., professor in the Department of Pediatrics at the University of California San Diego School of Medicine and Scripps Institution of Oceanography.
Each part of our body — including the gut, skin, mouth and nose — has its own set of microbes living in it.
Our microbiome and our health
We generally associate bacteria and viruses with getting sick. And sometimes, microbes do cause disease. The virus that causes the flu and the fungi that cause athlete’s foot are just a couple of examples.
But, the microbes in our microbiome can also be incredibly helpful — even essential — to our health.
Microbes help strengthen our immune system, fight certain pathogens (organisms that cause disease), digest food and turn it into energy, and absorb certain vitamins.
Researchers have found all kinds of associations between microbiomes and conditions ranging from Alzheimer’s disease and diabetes to colorectal cancer and obesity. And they keep investigating more.
One study found that people with more diversity in their microbiomes were more likely to sleep better and longer.
Other evidence suggests that our gut microbiome interacts with our brains, potentially affecting mental health and neurological conditions. Scientists don’t fully understand the gut-brain relationship yet, but studies in animals have shown that gut bacteria may reduce stress. And a 2019 paper in the journal Nature showed that the presence of certain bacteria in humans was associated with higher quality of life; lower levels of certain bacteria were associated with depression.
“The microbiome and the immune system are two sides of the same coin,” Gilbert said. “In fact the immune system evolved as a mechanism to manage the microbial garden in your body — like a gardener, the immune system helps to maintain the growth of bacteria that produce things we need and tries to eliminate the ones that may harm us.”
According to Gilbert, any disruption in the immune system or the microbiome can have an effect on the other, sometimes leading to autoimmune disease and allergies.
There is evidence that gut bacteria can actually prevent or improve food allergies, and other studies have shown that gut microbes can affect susceptibility to and severity of autoimmune diseases, such as rheumatoid arthritis and lupus among other autoimmune disorders.
The hygiene hypothesis
In an ironic twist, when we try to avoid germs — like when we douse ourselves or our kids in antibacterial hand sanitizer — we may actually be doing more harm than good.
The hygiene hypothesis is the idea that when an environment is too clean, our immune systems don’t learn to ward off infections as well as they could.
As the author of the book “Dirt is Good: The Advantage of Germs for Your Child's Developing Immune System,” Gilbert argues that most exposure to germs is good for kids and that parents should even give a pacifier that falls on the floor back to their baby without sanitizing it first.

But Gilbert also said it’s not too late for adults to get the benefits of exposure to diverse microbes.
“While early-life exposure can have profound impacts on the developing immune system, we believe that continual exposure to diverse sources of microbes throughout life still provides benefits,” he said.
Gilbert points to gardening as a way adults can diversify their microbiomes.
“We have found bacteria in soil that can have an anti-depressant effect through immune stimulation, as well as animal-associated bacteria that may improve lung function,” Gilbert said. “[This is] all very early work, but it points to potential benefits for adults, especially as you grow older.”
The indoor microbiome
Just like our bodies have a unique microbiome, so do our homes and workspaces. These indoor environments are called the indoor microbiome, which is made up of the same kind of microorganisms found in our bodies, such as bacteria and viruses.
In the “Wild Life of Our Homes” study, which analyzed household dust from more than 1,100 homes, researchers found that indoor microbiomes were more diverse than outdoor ones, influenced in part by who and how many people occupy the space.
If you’re a neat freak or a germaphobe dedicated to ridding your home of dirt, microbial diversity may sound like a nightmare when you realize it means many different types of bacteria, viruses and fungi are coexisting with you.
But it turns out, a little dust and dirt won’t necessarily hurt you, and it may even help you.
Take, for example, households with dogs. Dogs are notorious for sniffing everything and stepping in all kinds of substances outdoors, and then tracking that dirt inside.

But instead of trying to control the dirt your dog brings home from his or her routine walks, you may want to embrace it. Studies show that babies who interact physically with dogs have a 13% reduction in the likelihood of developing asthma. (Exposure to farm animals was even better.)
So should everyone get a dog to improve their microbial diversity and the protective qualities of their indoor microbiome? Gilbert might say yes.
“From a microbiome standpoint, [dogs] are a valuable source of immune simulation, as their bacteria activate our immune system and keep us healthy,” Gilbert said. “So yes, you should rescue a dog.”
So instead of shying away from a slobbery dog and hunting down all the dirt they bring in, consider the contribution the germs are making to your health. And instead of racing to beat the five-second rule if a piece of food falls on the floor, just eat it.
Your body will probably thank you.
- Colorful sweets may look tasty, but some researchers question ... ›
- 10 Signs You Have a Leaky Gut—and How to Heal It - HealthyWomen ›
- Gut Health and Brain Health. What's the Connection? - HealthyWomen ›
- The Wonderful World of Your Microbiome - HealthyWomen ›
- A healthy microbiome builds a strong immune system that could ... ›
- Colorful Sweets May Look Tasty, but Some Researchers Question Whether Synthetic Dyes May Pose Health Risks to Your Colon and Rectum - HealthyWomen ›
- A Healthy Microbiome Builds a Strong Immune System That Could Help Defeat Covid-19 - HealthyWomen ›
- How Menopause Affects the Gut Microbiome - HealthyWomen ›