March 21 to March 25 is National LGBTQ Health Awareness Week.
At age 28, Laura Silverstein tripped while running, dislocating her pinky finger trying to break her fall. Now 52, Silverstein said her experience at the emergency room that day still gives her “the heebie jeebies.”
The doctor probed Silverstein about her birth control method, and when she told him she was in a same-sex relationship, he asked invasive questions about her sexual orientation. When Silverstein, who identifies as bisexual, questioned why he was asking, she said the doctor appeared to get angry and defensive. All the while, Silverstein sat in pain as the ice she’d wrapped her finger in melted, dripping in her lap.
“What I needed from the healthcare system was prompt attention. I needed an X-ray, a pain killer, ice to reduce the swelling,” Silverstein said.
Instead, Silverstein got delayed care, undue suffering and a vague sense that she may have just experienced sexual harassment.
The incident had another lasting impact.
“That happened 23 years ago, and my pinky finger is still crooked,” Silverstein said. "I always wonder if I had had a better provider who treated me promptly and professionally if I wouldn't have to live with this visual reminder of sexual discrimination based on my sexual orientation.”
Silverstein’s experience is all too common.
According to the Center for American Progress (CAP) report, “The State of the LGBTQ Community in 2020, one in 10 LGBTQ people had experienced mistreatment from a healthcare provider (HCP) in the prior year.
Mistreatment may be overt — bullying, harassment or assault — or more subtle microaggressions, such as asking invasive questions unrelated to a patient’s care or not using a patient’s preferred pronouns.
A 2020 Kaiser Family Foundation (KFF) survey found that LGBTQ people were more likely than others to have had a negative experience with an HCP and twice as likely to feel their provider dismissed their concerns or assumed something about them without asking.
Dr. Sarah Pickle is a board-certified family medicine specialist and associate professor of family and community medicine at the University of Cincinnati College of Medicine, and she specializes in caring for transgender people. Pickle attributes these behaviors to implicit bias, societal cues and lack of training among HCPs.
Even seemingly small slights can harm patients.
“When somebody’s not using your chosen name and not using your pronouns, it demonstrates a lack of respect,” Pickle said. “It also makes individuals possibly wonder, ‘Am I safe here?’”
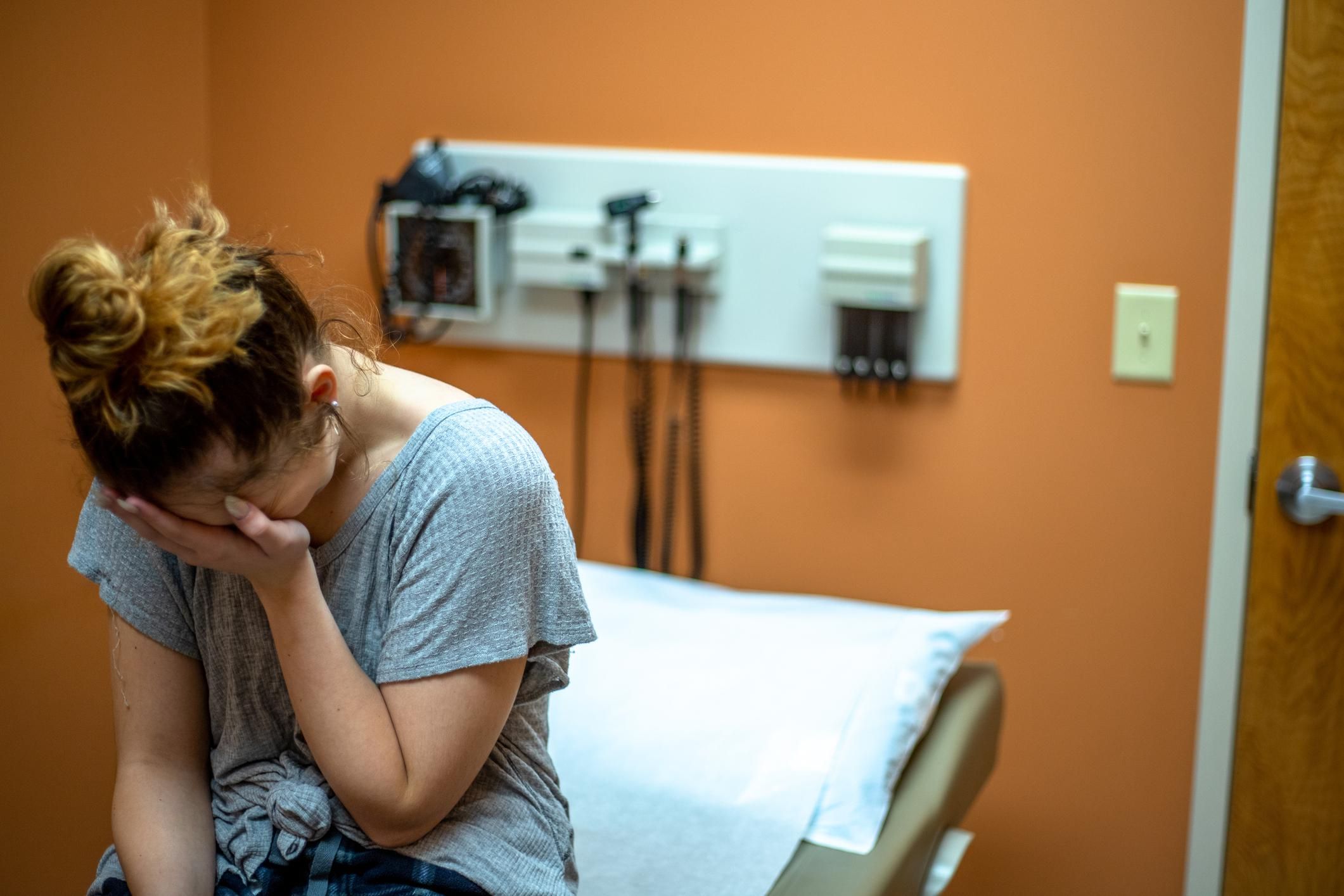
iStock.com/Elan Irving
Over time, chronic stress and fear of discrimination can negatively affect physical and psychological health. In fact, 20% of LGBTQ respondents in the CAP survey said they hadn’t seen a doctor to avoid discrimination and that number rose to almost half for transgender people.
The KFF survey also found that lesbian and bisexual women are less likely to seek preventive care, such as gynecological exams and mammograms, than non-LGBTQ women, putting them at risk for later diagnoses for health conditions, more expensive and extensive treatment, and worse outcomes.
Dr. Maria Monge, an adolescent medicine specialist and associate professor at Dell Medical School at the University of Texas at Austin, whose clinical practice focuses on caring for LGBTQ patients, said she has patients who avoided care for years. When they get to her clinic, many say they would have come sooner if they’d known they wouldn’t be judged for their gender identity or sexual orientation.
“It just speaks to how disenfranchised many minority communities feel by healthcare in general,” Monge said. “Building a space that is nonjudgmental and meets people where they are in terms of their healthcare needs really goes a long way to ultimately improving their health.”
Monge said LGBTQ people are not inherently sicker than others, but they face more barriers accessing healthcare that result in worse overall health. This could explain why, according to KFF, 23% of LGBTQ people feel their health is fair or poor compared with 14% of non-LGBTQ people.
Barriers are further compounded for LGBTQ people of color and members of other marginalized groups. Pickle noted that for a Black transgender woman who experiences racism and gender bias, layers of discrimination are additive and inseparable.
“LGBTQ equity has to happen aligned with racial equity and economic justice,” Pickle said. “It comes down to this idea that as individuals, we are complex. We hold multiple identities at the same time.”
Healthcare costs and coverage
Though 88% of LGBTQ people in the CAP survey have insurance, many still struggle with healthcare costs, like many Americans. More than one-quarter postponed or avoided care for illness or injury and 25% put off preventive screening because of cost.
Overall, 30% of LGBTQ people struggled to pay medical bills compared to 19% of non-LGBTQ respondents, and that figure was worse for LGBTQ women (35%) than for LGBTQ men (24%).
Even with health insurance, approximately one-quarter of LGBTQ people said their plan didn’t pay for a medical bill or a prescription they thought would be covered. Another 10% said insurance stopped covering a medication they were already taking.
Pickle said transgender patients commonly encounter these challenges when insurers change their policies and suddenly deny hormones patients have taken for years. Sometimes, insurance only covers a portion of gender-affirming surgery while denying aspects insurers deem cosmetic but that Pickle calls “lifesaving.”
The way forward

iStock.com/SolStock
To reduce discrimination against LGBTQ people, experts point to a multipronged approach, from training healthcare staff at all levels to laws protecting LGBTQ people from discrimination and policies enabling gender-affirming care.
Medical schools are increasingly offering training in transgender medicine, but Pickle said that alone won’t end implicit bias.
“Addressing one's ability to provide equitable care to gender-diverse folks and provide gender-affirming care — which is the ability to provide care that makes people feel comfortable and safe in their aligned gender — there has to be a continuous process of professional development,” Pickle said. “There's a lot of training that happens after formal training ends.”
Even small changes, such as removing gender-specific language on healthcare forms, can help, signaling that LGBTQ patients are welcome, Monge said.
Ultimately, healthcare providers need time and space to support their patients.
“It really is our responsibility as care providers to engage our patients in conversations about care, listen to them as the experts of their bodies, but not place the responsibility on them to teach us about the care that they need,” Pickle said.
Often, though, the responsibility does fall to patients, such as Silverstein.
“I now understand that a medical degree after someone's name does not automatically earn my trust,” she said. “I can say no to a doctor, or anyone, who is asking me to do or say things that feel wrong in any way.”
- Gender-Affirming Care Is Important ›
- Including LGBTQ+ People in the Menopause Conversation ›
- Danica Roem Is Transcending Gender - HealthyWomen ›
- Healthcare Access for Transgender Women - HealthyWomen ›
- Removing Barriers to Cervical Cancer Screening for the LGBTQ ... ›
- Embracing Hope: The Transformative Power of Gender-Affirming Care - HealthyWomen ›
- I’m a Pediatrician Who Cares for Transgender Kids - HealthyWomen ›







