Our editors sat down with Eleni Tsigas, executive director of the Preeclampsia Foundation, to find out more information about this common condition. To learn everything you need to know about preeclampsia, read her answers below.
What is preeclampsia?
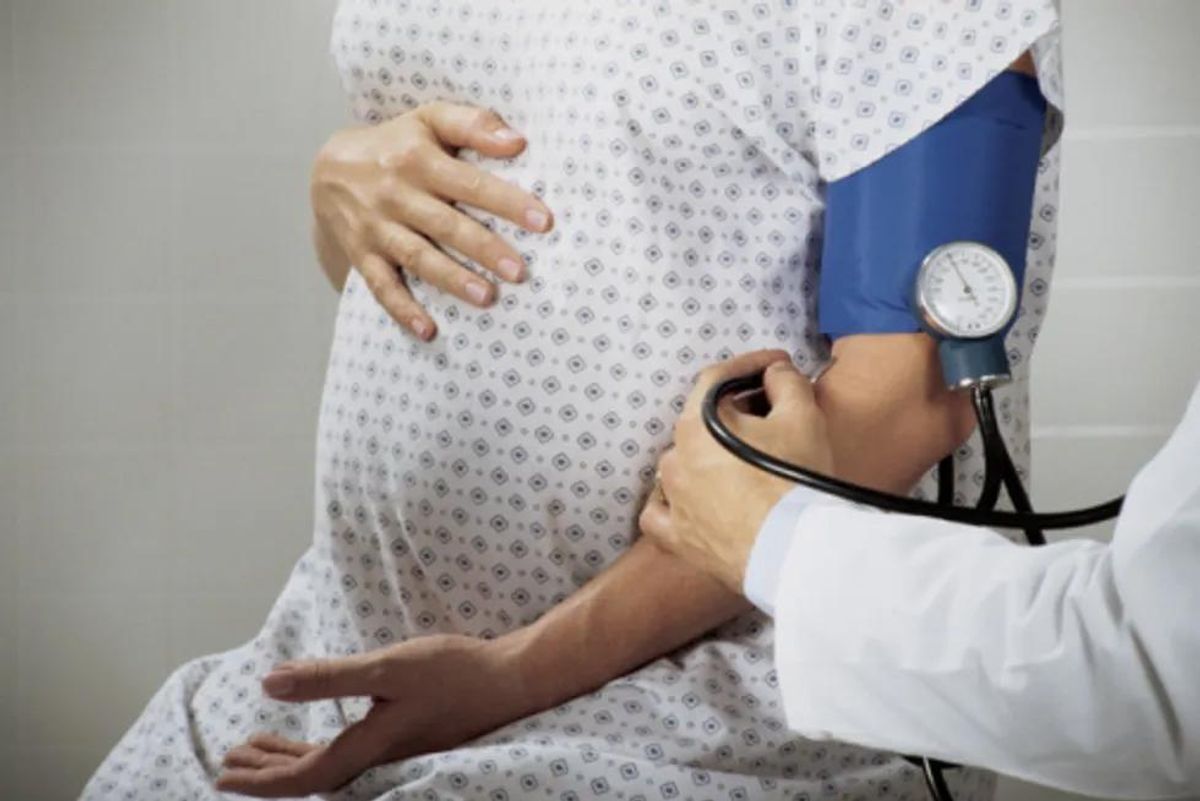
Preeclampsia is a disorder that occurs during pregnancy and is characterized by high blood pressure in the second or third trimester of pregnancy. It affects about 5 to 8 percent of pregnancies in the United States. Several conditions or factors may lead to preeclampsia, but scientists have not pinpointed the cause. Studies have looked at autoimmune disorders, blood vessel issues, poor diet and genetics, but results are inconclusive.
Although all women are at risk, those who are obese, pregnant for the first time, expecting multiples, older than 35 or have a history of diabetes, high blood pressure or kidney disease have a higher risk of developing preeclampsia.
As with most conditions, early detection of preeclampsia may lead to better treatment, and knowing the signs and symptoms is key to prompt diagnosis. Keep in mind that not all women will experience illness or severe effects of the condition, but preeclampsia, which can be quite serious, can develop into eclampsia—seizures that are not related to a preexisting brain condition. If you are at high risk for preeclampsia, discuss your risks and diagnosis with your health care professional.
Does preeclampsia have recognizable symptoms?
While many pregnant women experience swollen feet, swelling in the face and hands, as well as sudden weight gain, these can be signs of preeclampsia. Talk to your health care professional about getting tested for preeclampsia if you have those or other possible symptoms of preeclampsia, such as:
- persistent headache
- stomach or chest pain
- irritability
- decreased urination
- nausea
- vomiting
- changes in vision
If you receive a diagnosis for preeclampsia, your health care professional can monitor your baby's well-being with a fetal ultrasound and a non-stress test.
How is preeclampsia treated?
Although delivery of your baby is the only way to treat preeclampsia, your doctor may decide to monitor your pregnancy more closely in the hospital or, if your preeclampsia appears to be very mild, at home, until your baby has a good chance of a healthy delivery. Your doctor may recommend:
- bed rest, primarily lying on your left side
- drinking plenty of water every day
- frequent checkups to make sure you and your baby are doing well
- medicines to help control your blood pressure (sometimes)
If any of your symptoms worsen or you have new symptoms, immediately notify your doctor. You may also be treated at the hospital with medicines given into a vein to control blood pressure and prevent other complications. Depending on the age of your baby, you may receive steroid injections to speed the development of your baby's lungs.
If your preeclampsia is severe, the doctor may decide to deliver your baby early, especially if your baby is not doing well in the womb or your blood pressure gets too high. Normally, your doctor will try to wait until the 37th week of pregnancy.
Will the condition have long-term effects for my health and that of my baby?
Babies born prematurely to mothers with preeclampsia may experience problems. Occasionally, the mother may also experience serious complications, including bleeding problems, premature detachment of the placenta from the uterus, liver rupture or stroke. Death of the mother from preeclampsia is rare in the United States.
In most cases, blood pressure readings return to normal by six weeks after you deliver, though they can spike during the week after giving birth. Once you've had preeclampsia, you are at risk of developing the condition during subsequent pregnancies.
Studies show that women with a history of preeclampsia are at four times the risk of developing high blood pressure and twice as likely to have ischemic heart disease, heart attack and stroke later in life.
Even without loss of the child, in severe cases of preeclampsia, women and their family members can be emotionally traumatized. Counseling is recommended, along with support from others who have had similar experiences.
What can women do to improve birth outcomes from preeclampsia?
Expectant mothers can be aware of warning signs so as to report them promptly and advocate for themselves as empowered, knowledgeable women. But for all women who care about the health of mothers and their babies, raising awareness of this condition via any of the ideas posted on the Preeclampsia Foundation's Get Involved page or join in a local Promise Walk for Preeclampsia will directly help us with the ultimate goal of removing preeclampsia as a threat to pregnant women.
- 33 Weeks Pregnant: You May Start to Have Trouble Breathing ›
- Signs You're About to Faint - HealthyWomen ›
- Life after HELLP syndrome - HealthyWomen ›