Osteoporosis is a medical condition that causes your bones to become brittle and fragile as a result of losing bone tissue, and it's one of the most common health conditions that women experience. In fact, one in two women will break a bone in their lifetime as a result of the disease. That makes it a far higher risk than for breast cancer, heart attack and stroke — combined. And women are far more likely to develop osteoporosis than men.
We asked Nicole C. Wright, M.D., director of education of CHOICES at Tulane University, for some questions about osteoporosis to ask your healthcare provider (HCP).
What causes osteoporosis to develop?
Simply put, osteoporosis develops when bones break down faster than they grow. There are three types of cells in our bones: those that are responsible for forming bones, those responsible for breaking down bones, and those that help the other two types of cells and other cells throughout the body talk to each other.
In childhood, the cells that form bone grow faster than the cells that break down bone. But after menopause (either surgical or natural), the cells that break down bone grow faster than the cells that form bone.
Why is osteoporosis more common in women?
Osteoporosis is more common in women because of the role estrogen plays in bone health. Estrogen tells the bone formation cells to form new bones. Once we lose estrogen during menopause, these cells no longer get these signals, and no new bone forms. Since bone continues to break down as always, your bone density decreases.
What tests are used to evaluate bones?
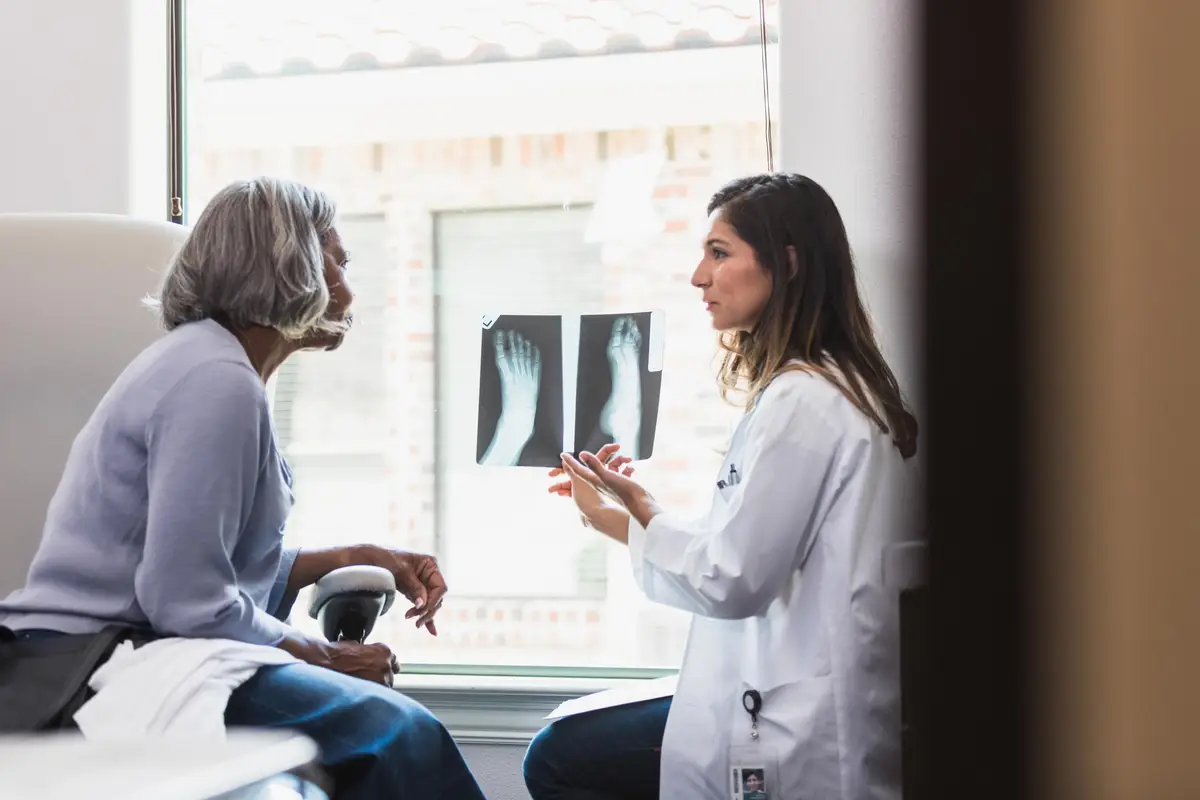
The primary test used to evaluate bones is the DEXA (or DXA) scan, which stands for dual-energy X-ray absorptiometry. It measures bone density and compares it to a young adult population of the same gender and ethnic background — called a reference population — to calculate a T-score, which HCPs then use to diagnose osteoporosis. Other machines, such as ultrasound, particularly at the heel; traditional X-rays; and computed tomography (CT) scans, have the ability to measure bone health, but diagnoses aren't made from these images.
At what age should I start thinking about my bone health? Or having a bone density test?
It's never too early to think about bone health.
- Birth to late 20s — early growth stage: During this time, children must receive proper nutrition and activity so they reach their genetically determined peak bone mass.
- Late 20s to menopause — maintenance stage: Adults should continue eating well and exercising to maintain bone health. If you have any health conditions that may have a negative impact on your bone health, such as thyroid disorders, celiac disease or rheumatoid arthritis, be mindful of them and talk to your HCP about what you can do.
- Menopause and beyond — the aging process: This is when most people start thinking about bone health. But, unfortunately, bone loss has already begun by then. National guidelines recommend that women start getting DXA scans at 65, but they can get one earlier if they have health conditions that increase their risk for fractures.
How can I prevent falls and fractures?
There is so much you can do to prevent fractures. First, learn what factors in your life increase your risk. Find out whether you're on medication or have a health condition that has been associated with fracture risk. Then assess your lifestyle and nutrition. Make sure you're doing the appropriate exercises to strengthen your bones and improve your balance. These include strength-training exercises, particularly those for the upper back; walking; low-impact aerobics; and stair climbing. Learn which foods contain helpful amounts of calcium, vitamin D and magnesium — like low-fat dairy products, salmon and spinach — and add them to your diet. Finally, evaluate your fall risk. Fall prevention can be based on improving your muscle strength and balance, or it can be environmental, such as removing trip hazards, assessing vision problems and wearing proper shoes.
What changes can I make to my lifestyle to reduce my risk?
In addition to improving your nutrition and exercise routine, you should also stop smoking if you're a smoker. Nicotine interferes with estrogen's role in the bone formation cells, and other toxins in cigarettes are harmful to the blood vessels in the bone. People who smoke at an early age often do not reach their peak bone mass, and studies have found that smokers have more recurrent fractures than non-smokers and an earlier menopause.
You should also do your best to lower your stress level. Experts have found a connection between stress and osteoporosis.
Does my calcium or vitamin D intake affect my risk for osteoporosis? What are some supplements I can take?
Calcium is an important nutrient for every cell in the body. It is found in foods such as kale, collard greens, sardines, salmon, dairy products, and fortified cereal and orange juice. If you do not have enough, your body will take it from your largest calcium storage unit: your bones. If your diet does not provide 1,000 mg of calcium daily (1,200 mg if you are over 51), you should take supplements. Calcium citrate supplements don't need stomach acid to be absorbed by your body and can be taken at any time of day, but pick a supplement that works best for you.
You can't absorb calcium without its good friend, vitamin D. Luckily, you can get vitamin D from foods such as fatty fish; cheese; egg yolks; and fortified juice, cereal and dairy products, as well as from spending a small amount of time in the sun each day. If you're not getting 800 IUs of vitamin D naturally per day, you should supplement with a vitamin D3 pill.
If I have a family history of osteoporosis, does this put me at higher risk?
Although osteoporosis is not a fully genetic disease, you are at higher risk of developing osteoporosis and fractures if you have a family history of osteoporosis, particularly a family history of hip fractures.
Are there any ways to prevent my osteoporosis from getting worse?
Osteoporosis is not something that you can prevent from getting worse as you age. For those with low bone mass, changing your diet and exercise regimen could be the tool that improves your bone health. However, those further along in the bone-loss spectrum may need medicine. There are several approved medications for the prevention and treatment of osteoporosis that also reduce the risk for fractures. Some of these medications are associated with rare, yet serious, side effects, so it is important to have a discussion with your HCP to make an informed decision about using them.
What are some available resources/treatment options to help me cope with my osteoporosis?
There are many patient resources regarding osteoporosis. The National Osteoporosis Foundation and American Bone Health websites are good places to start.
This resource was created with support from Amgen.
- Fast Facts: 10 Facts About Osteoporosis in Women - HealthyWomen ›
- Osteoporosis and Fractures: What You Should Know - HealthyWomen ›
- What You Need to Know About Osteoporosis - HealthyWomen ›
- Menopause and Osteoporosis: How to Take Charge of Your Bone Health - HealthyWomen ›
- Osteoporosis: Knowing – and Owning – Your Numbers - HealthyWomen ›
- The Osteoporosis and Depression Connection - HealthyWomen ›
- How To Avoid Falls in Your Home - HealthyWomen ›
- Risk Factors for Bone Fractures and Osteoporosis - HealthyWomen ›
- Osteoporosis Is a Looming Public Health Crisis - HealthyWomen ›
- I Discovered I Had Osteoporosis When I Broke My Elbows - HealthyWomen ›
- Descubrí que tenía osteoporosis cuando tuve fracturas en mis codos por una caída - HealthyWomen ›
- Facts About Women’s Bone Health - HealthyWomen ›
- Osteoporosis Treatments - HealthyWomen ›
- Tratamientos de la osteoporosis - HealthyWomen ›
- I Have Postmenopausal Osteoporosis - HealthyWomen ›
- My Broken Wrist Was a Red Flag that I Was Losing Bone Mass - HealthyWomen ›
- Mi muñeca rota fue una señal de alerta de que estaba perdiendo masa ósea. - HealthyWomen ›