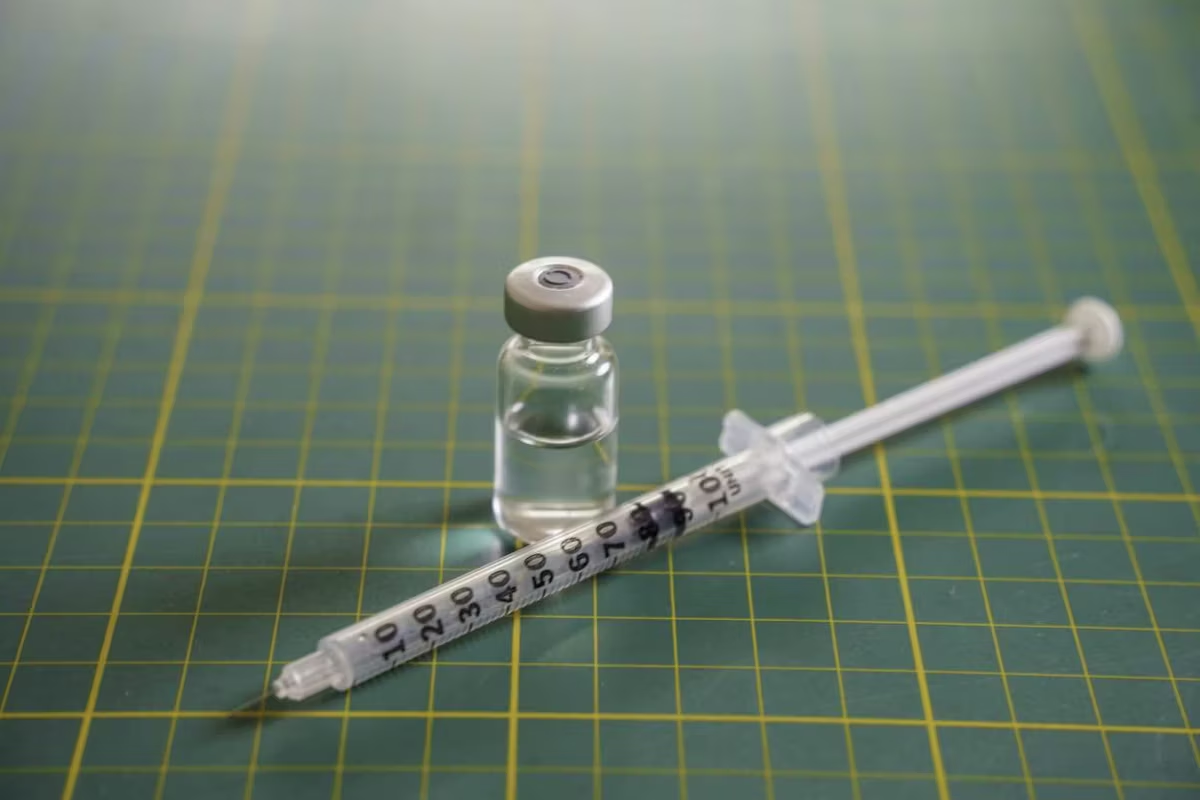
GLP-1 medications are everywhere these days — especially online.
A quick scroll through social media can bring up a wide range of companies and influencers touting the benefits of GLP-1 drugs, and women tend to be the target audience. A recent study in the Journal of Medical Internet Research found most of the posts about GLP-1s highlighted positive benefits for women’s health. And while it’s true that GLP-1 drugs have proven benefits for some people, not all GLP-1 medications are the same. And not everything you’re reading online is true.
The difference between FDA-approved GLP-1s and compounded GLP-1s
Glucagon-like peptide-1 (GLP-1) medications are prescribed to treat and manage Type 2 diabetes and obesity. The medications help control blood sugar, slow digestion and increase fullness, which all help with weight loss.
Commercial GLP-1s (brand names Ozempic, Wegovy, Mounjaro and Zepbound) are regulated by the Food and Drug Administration (FDA) for safety, quality and effectiveness. They undergo rigorous FDA review, clinical testing and manufacturing inspections before being approved for use. But many of the GLP-1s advertised on the internet are compounded GLP-1s, which means the drugs are made in compounding pharmacies, and the products are not approved by the FDA or regulated in the same way as the branded versions.
Compounded GLP-1s serve a limited role when they are used to accommodate specific patient needs, such as an allergy to an ingredient or difficulty swallowing a pill, that cannot be met by an FDA-approved drug. Compounding is also permitted to boost supply during a drug supply shortage. This is what happened when there was a shortage of commercial GLP-1s shortly after they first became available for treating obesity. But the shortage has since ended, and the FDA ordered compounders to stop manufacturing mass-compounded GLP-1 drugs in early 2025.
Risks associated with mass-produced compounded GLP-1s
Although the FDA has declared that the supply shortage is resolved, some companies continue to mass produce compounded versions of GLP-1s, claiming that the drugs are personalized for patient needs by altering the method of delivery (e.g., gummy, injection, spray) or adding unnecessary and unproven ingredients like B12 and glycine. In some cases, products marketed as compounded GLP-1s by bad actors have been found to be counterfeit or to contain ingredients other than what is advertised — meaning they may not even be real GLP-1 drugs at all.
The risks of taking any compounded GLP-1s include:
- Medication that contains too little or too much of the active ingredient
- A product that contains no active ingredients at all
- Dosing errors when taking the medication
- Adverse reactions
How to be a smart consumer when it comes to compounded GLP-1s
Compounded GLP-1s can vary in strength, effectiveness and quality, so they should only be taken under the guidance of a healthcare provider (HCP). Staying informed and asking the right questions can help you protect your health and avoid unnecessary risks.
Here’s how to be a smart consumer:
- Consult with your HCP before taking anything new: Checking in with someone who knows your health history is always a good idea when thinking about taking a new medication.
- Check out the pharmacy: Legit compounding pharmacies are licensed by the state. Make sure the pharmacy has a physical U.S. address and phone number, and a licensed pharmacist you can talk to. You can check the pharmacy through the National Association of Boards Pharmacy.
- Ask questions about what you’re taking: Compounded GLP-1 medications may include supplemental ingredients such as vitamin B12 and glycine. As of this time, there are no studies that support that there is any benefit or effectiveness of supplements or the personalization of GLP-1s.
- Know the FDA-approved forms of medication: Oral drops, gummies, patches and sprays are fraudulent forms of GLP-1s and are not FDA-approved.
- Know what ingredients are approved by the FDA: Research common ingredients such as semaglutide sodium and acetate used in compounded alternatives, as well as terms like “microdose,” and whether FDA-approved data for those ingredients is available.
- Avoid products that seem too good to be true: FDA-approved products are required to use advertising that’s truthful, balanced and not misleading, so if you’re seeing claims that don’t seem realistic, take a second look. Companies may pay influencers to post dramatic before-and-after photos and testimonials that aren’t true or make claims that the compounded formulas are regulated by the FDA. Companies may also use AI to create deep fakes to make their claims seem credible.
- Report any issues with compounded GLP-1s: Packaging with misspelled words, inconsistencies or written in a language other than English are most likely a scam. Most legit products will have serial/lot numbers that can be verified. Call your pharmacy or HCP with any concerns. Side effects and dosing issues should be reported to the FDA’s MedWatch
.
Know what you’re getting when choosing a GLP-1
Compounded GLP-1s are often promoted as personalized medicine, but they come with risks that should be navigated carefully. Illegitimate companies and counterfeit products are harmful to consumers.
All women deserve safe, effective treatments. Advocating for yourself — and choosing an FDA-approved drug when possible — are key to finding quality medications to treat any health condition.
This educational resource was created with support from Eli Lilly, a HealthyWomen Corporate Advisory Council member.