This article has been archived. We will no longer be updating it. For our most up-to-date information, please visit our pain management information here.
It must have been that super-strenuous spin class I took last week, when my mind fooled me into believing I was 35 but my body stubbornly acted its age. Energized but exhausted, I continued this self-deception by joining a friend after class in some challenging new ab work. She showed me new moves she'd recently learned. I struggled to keep up with her, but my body protested until I graciously bowed out.
What happened the next day wasn't pretty. The minute I got out of bed I knew something was wrong. Pain shot through my right leg and then the leg buckled, threatening to throw me to the ground. And at frequent intervals throughout that day, that strange sensation threw me into fits of grimacing and grabbing onto the closest thing within reach to steady myself. Fortunately, I was in my house working, and no one except my dog could see my twisted expressions (and it didn't seem to faze her one bit—she's old; what can I say?) Except, that is, when hubby returned from work that night. "That's just not normal!" he said, the first time he witnessed my sudden near-collapse. "There's something wrong!" he insisted.
I figured I'd injured myself the day before and this is what I got … but then I guess his worry became contagious and suddenly seized my more sensible thoughts. Nasty contemplations ran through my head: A blood clot? Some rare neurological disease? A bone/circulation/muscular disorder?
I called my doctor the next day and described what was happening. "It's most likely your lower back," he said. "That's common." I decided to wait a few days for it to improve. And the next morning, when I got out of bed, my lower back was sore—but the leg only buckled once or twice. And by the day after that … voila! My leg stayed as steady as the proverbial rock.
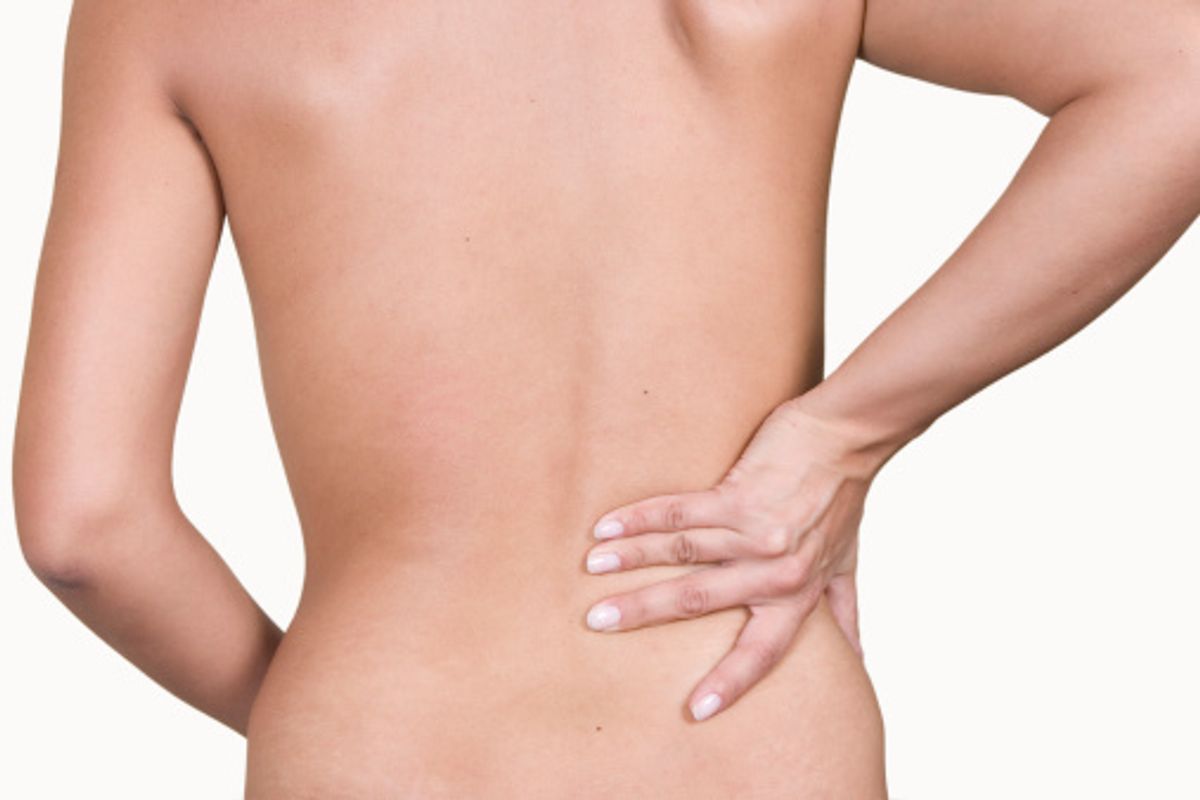
I'm sure you can relate to lower back pain; if you can't, you're in the minority. Up to 80 percent of us experience it at one point or another. It's so prevalent that it is estimated to cost Americans at least $50 billion each year in the quest for relief, and comes in second (behind headaches) as the most common neurological complaint in the United States.
Fortunately, I'm pretty much on the mend now, my back feeling (almost) back to normal. But I realize I'm lucky: many lower back aches take much longer to go away. Mine was caused by a sports injury, most likely pushing myself beyond my limit for that day, or positioning myself incorrectly on the bike. Others might experience back pain after lifting something too heavy, gardening or an event as innocent as sneezing, coughing or just turning around too quickly. Or a degenerative condition like arthritis may be to blame. And then there's always another cause—that "A" word. Aging. Our bone strength and muscle tone elasticity decrease with age; discs begin to lose their cushioning fluid and flexibility.
But back pain does not have to equal surgery. Most people do recover, in time, with some self-care.
Ice or heat: Compresses may help reduce pain and inflammation. Time matters: As soon as possible, apply a cold pack or cold compress to the tender spot for up to 20 minutes several times daily; a bag of ice or even a bag of frozen peas wrapped in a towel will work. After two to three days, switch over to heat to relax muscles and increase blood flow to the area. And there's nothing more soothing than a warm, relaxing bath.
Rest: I remember long ago when bed rest was the standard treatment for back pain. I don't know about you, but I feel much better when I'm up and about; things seem to stiffen up when I sit or lay flat. And studies have backed that up, finding that people who continue with their activities tend to appear to have better back flexibility than those who rested in bed for a week. Caution: there are some instances where rest is necessary and the preferred treatment. And when you do rest, lying on your side with a pillow between your knees can take some of the pressure off your muscles; or try lying on your back with a pillow beneath your knees.
Exercise: Gentle exercises can speed recovery and keep flexibility at its peak. This may include swimming, walking and movement therapy, which can develop better posture and coordination. Yoga and gentle stretching also might be effective ways to manage lower back pain. And there's a lot to be said, psychologically, for feeling like you're in control and actively doing something to help yourself. (Don't get overzealous, though: If you feel pain that goes beyond mild and lasts more than 15 minutes during exercise, stop what you're doing. Don't push yourself to do something that causes even more pain. Stay within your limit and listen to your body.)
Alternative treatments: Needles may sound scary, but these tiny, hair-thin flexible needles (in fact, it's hard to really call them "needles" in the conventional sense) can trigger the release of endorphins, the body's naturally occurring pain relievers. Acupuncture dates back centuries, but studies have shown it to be superior to medications or physical therapy in treating chronic back pain. Although acupuncture is controversial among many Western scientists and physicians, others support it. The WHO (World Health Organization) has found it effective in treating 28 conditions.
In addition, some people (about 22 million Americans visit them annually) swear by chiropractors, who gently manipulate and align the spine and may also incorporate other treatments such as ultrasound, massage, biofeedback and nutritional therapy.
Therapeutic touch and Reiki are "energy-based" techniques that don't involve direct physical contact. They are thought to help activate the body's own self-healing capacities. The jury is mixed on their efficacy, though, for many, they may help ease the anxiety associated with pain and thus might relieve muscle spasms associated with stress.
Medications: Many people find they are able to manage their pain with over-the-counter remedies like ibuprofen, aspirin or naproxen. Prescription drugs like muscle relaxers, opioids, anticonvulsants and even some antidepressants are sometimes recommended to manage moderate to severe pain. (But please remember to always check with your doc before taking drugs to manage pain; even over-the-counter medications can be unsafe in certain instances and can conflict with other medications or herbal supplements you might be taking.)
And then, there's more: More approaches to treat back pain include injections of local anesthetics, steroids or narcotics into affected areas; traction, TENS (transcutaneous electrical nerve stimulation) and ultrasound.
Spinning class will have to do without me for now, although I must admit, I miss the challenge. Perhaps the next time I go, I'll forgo the after-class exercises with my friend and instead use that time for some gentle stretching and catching up.
You might also want to read:
Chronic Pain: Move It to Lose It