Ouch! Just rubbing your breasts the wrong way is painful. Your mind starts racing. You worry that you have cancer. Or maybe you fret that your contraception wasn't doing its job and maybe this is an early sign of pregnancy.
Breast pain is rarely something to worry, panic or be alarmed about. Here are just a few reasons why you may have sore breasts.
When in doubt, reach out to your health care provider to help figure out what's going on.
1. You're getting your period.
It's totally normal to have breast tenderness and swelling right before the onset of Aunt Flo. It can happen for up to a week and you can have so much swelling that your bra size might change. Once your period starts, your breast size will return to normal and the tenderness will gradually subside. Why does this happen? Estrogen causes your breast ducts to get bigger. And progesterone increases the growth of your milk glands. Find out about period weight gain.
2. You're pregnant.
Bust out the nonalcoholic champagne—you're having a baby! Thanks to your hormones, breasts that are tender, sore, achy and swollen are often the first sign you're pregnant. Early on in pregnancy, your breasts grow faster than your baby. As your estrogen levels rise, they increase the size of your milk ducts. And that can boost breast sensitivity and pain. If you have breast pain and have missed a period, take a pregnancy test to confirm if you've conceived. Read more about early pregnancy symptoms.
3. You're breastfeeding.
When you're pregnant, your milk ducts and breasts get larger so that you can breastfeed. (That's why some pregnant women have crazy cleavage!) You may be in pain thanks to that growth. It continues once you're breastfeeding and baby is sucking on your breasts nonstop. Contact a lactation consultation who can help you find a less painful breastfeeding technique. If you're ready to stop breastfeeding, find out how to wean your child from breastfeeding.
4. You're taking certain meds.
Some medications trigger breast pain. Those medications include certain diuretics, digitalis preparations, methyldopa (Aldomet, for high blood pressure), spironolactone (Aldactone, for high blood pressure), oxymetholone (Anadrol, a powerful oral steroid) and chlorpromazine (an antipsychotic). If your breasts are uncomfortable and meds are to blame, your health care provider may be able to prescribe another medication.
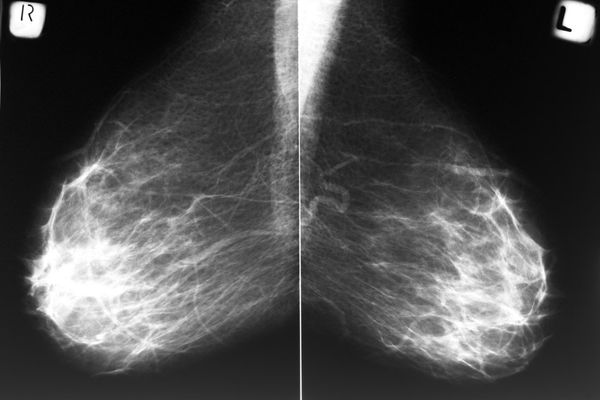
5. You have breast cancer.
Don't worry yet that it's the "C" word. Most people who have breast pain don't have cancer. It's still a valid concern, though. If you're feeling pain, speak with your health care provider. Review your breast cancer risk factors and tell your provider if you've noticed any other changes in your body such as bloody or clear discharge from your nipple; a lump in your breast; or local redness, pus or fever. Your health care provider will decide if you should go for a mammogram or get other testing to dig further into what's going on.
6. You need a new bra.
Has your favorite bra seen better days? Maybe the underwire is stabbing you. It doesn't fit anymore. The fabric is itchy. Your boobs just hurt by bedtime. It's time to invest in a few new supportive bras for the sake of your comfort and breast health. You don't want one with shoulder straps digging into your skin or the back is riding up or where your breasts are coming out of the cups. A professional bra fitter can measure you and help you choose one that's right for you. (And get a properly fitting sports bra while you're there, too.)
7. You've experienced breast trauma.
Maybe you had a procedure done on your breasts. Or a basketball landed right on your boobs. These types of traumas can leave you with sore breasts. Most pain from such issues should go away quickly. Speak to your health care provider if pain persists to make sure you didn't crack your ribs or are dealing with scar tissue issues.
8. You're allergic to fragrant products.
Some chemicals can cause allergic reactions like pain, redness, inflammation and swelling. Culprits include moisturizers, laundry detergents (because clothing rubs your skin), sunscreens, cosmetics and hair products (they get on your chest when you bathe). Think about whether you've added a new product to your beauty regime. Remove it from your routine and see if the pain disappears.
9. You exercised too much.
Did you do extra pushups in your last class? Did you go for a long run in your old sports bra? Some exercises and the intensity at which you do them can strain your chest wall's muscles. It can be hard to differentiate between breast pain and chest muscle pain because the two are so similar. If the pain goes away after you've skipped workouts and taken some over-the-counter pain relievers, you may just be dealing with a muscular issue. Learn more about post-workout breast pain.
10. Your hormones are on the fritz.
Anything that affects your hormones can cause breast pain. Some culprits include fertility treatments, hormone replacement therapies, thyroid medications and birth control pills (even switching birth control regimens). These can cause sensitivity, tenderness and swelling because they impact your estrogen levels. The side effect of breast pain will lessen over time; your body needs time to adjust to the new surge of hormones. Speak with your health care provider to see if you need to switch anything in your health care regimen.
11. You have fibrocystic breasts.
When you have fibrocystic breasts, you have multiple cysts throughout both breasts. Your breasts can feel tender, swollen or painful because their tissue is lumpy or rope-like. And your symptoms don't come and go with your menstrual cycle. While fibrocystic breasts are noncancerous, your health care provider will still want to monitor them.
12. You have an infection.
If you have an infection, you'll have breast redness, swelling and pain. Your nipple(s) may be leaking blood, pus, or brown, green or red discharge. You may be running a fever. Infections can be caused by factors such as ingrown hairs, clogged sweat glands or blocked milk ducts. Your health care provider can figure out what's going on. Many infections can be treated with antibiotics.
- Early Pregnancy Symptoms Before You Miss Your Period ›
- Perimenopausal Breast Tenderness ›
- 4 Things That Pain in Your Left Boob Might Mean ›
- Breast Pain and Menopause ›
- As a Breastfeeding Mom Who Also Worked as a Lactation Consultant, I Thought My Breast Lump Was a Clogged Milk Duct - HealthyWomen ›