What is thyroid eye disease (TED)?
Thyroid eye disease, or TED, is an autoimmune disorder that causes inflammation in the eye muscles, eyelids, tear glands and fatty tissues behind the eye. TED is sometimes called Graves’ ophthalmopathy or Graves’ Eye Disease. This is because TED most often occurs as part of Graves’ disease — an autoimmune condition that causes your immune system to attack the healthy tissue of your thyroid, skin and eyes.
If you have Graves’ disease, you have an increased chance of developing thyroid eye disease. But TED is a rare disease and different from Graves’ disease and requires different treatment. Graves’ disease is the most common cause of hyperthyroidism, where your body produces too much thyroid hormone. TED can also occur with hypothyroidism, where your body produces too little thyroid hormone, but this is much less common. When thyroid hormone levels go up and down, it can make your TED symptoms worse. Thyroid eye disease is more common in women, but is often more severe in men.
Phases of thyroid eye disease (TED)
There are two phases of TED: active (also called acute) and inactive (also called chronic). TED begins with an active phase where you suddenly begin to experience symptoms. This phase can last from about 6 months to 2 years. During the inactive phase, most of the symptoms tend to get better, but this is only temporary. Scar tissue can form in the eyelid and eye muscle during the inactive phase.
What can make thyroid eye disease (TED) worse?
Certain factors can trigger symptoms or cause flare-ups.
- Smoking
- Fluctuating hormones, such as in pregnancy
- Stress
- Eye trauma or surgery
- Other autoimmune conditions such as Type 1 diabetes, lupus or rheumatoid arthritis
- Steroid use
What are the symptoms of thyroid eye disease (TED)?
TED is a serious disease that can get worse over time. Most people who have a thyroid condition such as Graves’ disease start noticing eye symptoms within the first 6 months. These symptoms can include:
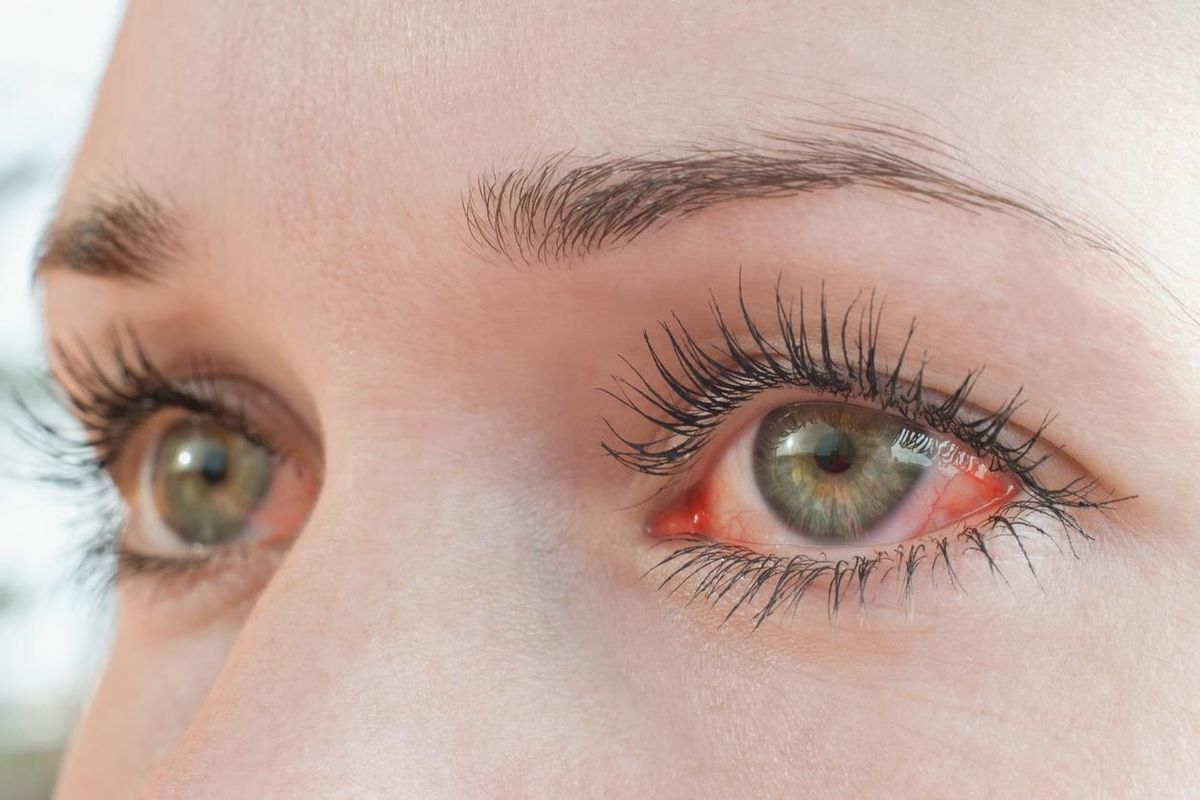
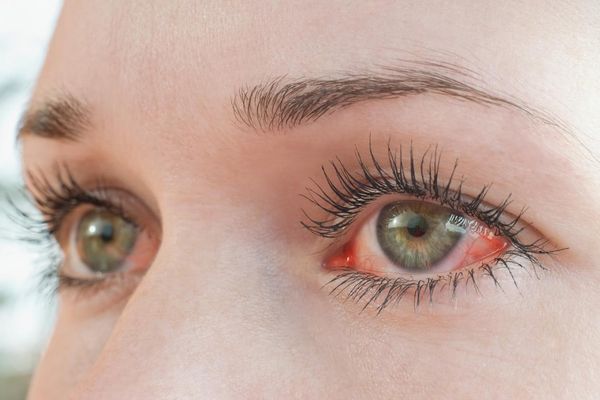
- Dry, itching or gritty eyes
- Eye tearing or redness
- Pain behind the eye
- Puffy skin around the eyes or eyelid swelling
- Double vision
- Misaligned eyes or eyes that don’t work together
- Bulging eyes (proptosis or exophthalmos)
- Sensitivity to light
You might also have more severe symptoms such as not being able to move your eyes or eyelids well, not being able to completely close your eyes or, in rare cases, loss of vision. This can affect quality of life because it can affect your ability to drive, read and work and can impact your emotional well-being.
How does thyroid eye disease (TED) get diagnosed?
Sometimes your HCP can make a diagnosis of TED based on your symptoms alone. To get a diagnosis of thyroid eye disease, you will need a physical exam, as well as an eye exam. You might also have blood drawn to check the status of your thyroid, along with vision tests and eyelid measurements.
It might take visits to more than one HCP to get a TED diagnosis. You may be referred to see an ophthalmologist who is a doctor that specializes in eye and vision concerns, specifically a thyroid eye disease specialist with advanced training and experience treating TED. A referral to an endocrinologist, who is a doctor that treats hormone issues, might also be recommended to help you manage your thyroid condition.
Sometimes the symptoms of TED such as dry, red and irritated eyes can be mistaken for allergies. Tell your HCP about all your symptoms and medical history, so there is not a delay in diagnosis.
Managing thyroid eye disease (TED) symptoms
While TED isn’t considered to be curable, there are treatments that can help manage your symptoms. The longer that TED remains untreated, the more likely serious damage can occur. Treatment is often started in the acute phase, but can still help during the chronic phase.
At home, you can use cool compresses or lubricating eye drops to give your dry or irritated eyes some relief. Sunglasses can help protect your eyes from the sun and wind. To help with the swelling and pressure near or in your eyes, try sleeping with your head elevated.
Certain medications can help with eye swelling, such as steroid medications. There are also newer prescription infusions available that may help relieve symptoms.
If your TED symptoms are severe, your HCP might recommend you have surgery. Orbital decompression can be performed if you’re experiencing bulging eyes. This surgery helps make the eye socket bigger to decrease the pressure in your eyes. Eyelid surgery can also be performed if your eyelids have pulled back too much. This helps return them back to their normal position.
If you are concerned that you might have thyroid eye disease, talk with your HCP. They can work with you to come up with a treatment plan that will work for you.
This resource was created with support from Horizon.
- Fast Facts: Everything You Need to Know About the Thyroid ›
- Thyroid Awareness: What Happens When This Little Gland Goes Haywire ›
- Thyroid Disorders Hub - HealthyWomen ›
- 15 Things Your Thyroid Can Affect ›
- The Phases of Thyroid Eye Disease - HealthyWomen ›
- Questions to Ask Your HCP About Thyroid Eye Disease - HealthyWomen ›