Susan Christian had never been a good sleeper, so when her sleep got increasingly worse during her 40s, she chalked it up to aging. It wasn't until she turned 50 and started waking up gasping — desperately — for air that Christian decided to get help and was eventually diagnosed with sleep apnea.
Although it's true that many women have trouble sleeping soundly as they get older, especially during menopause, you shouldn't assume disruptions like snoring and restless sleep are normal. They could be signs of sleep apnea, a potentially serious sleep disorder.
What is sleep apnea?
Sleep apnea is characterized by abnormal breathing during sleep, and people with sleep apnea take long pauses between breaths while sleeping.
There are three types of sleep apnea.
- Obstructive sleep apnea is caused by repeated closure of the throat or upper airway during sleep and is the most common type of sleep apnea.
- Central sleep apnea is much rarer and is caused by a problem with the part of the brain stem that controls breathing.
- Mixed sleep apnea is a combination of central and obstructive sleep apnea.
Between 2% and 9% of adults are estimated to have obstructive sleep apnea, with many more cases going undiagnosed.
Signs and symptoms of sleep apnea
The most common signs of sleep apnea are snoring and feeling tired no matter how much sleep you get. Women tend to report symptoms like unrefreshing sleep, fatigue, insomnia and depression, says Dr. Smita Patel, an integrative neurologist and sleep medicine physician at the iNeuro Institute who is a member of HealthyWomen's Women's Health Advisory Council (WHAC). Other symptoms include:
- Waking up with a dry mouth or sore throat
- Headaches
- Trouble staying awake during the day
- Difficulty concentrating
- Frequent nighttime waking
Note that snoring doesn't mean you have sleep apnea — nearly everyone snores now and then. But it's important to bring up snoring with your healthcare provider (HCP), especially if you're experiencing other symptoms of sleep apnea.
How is sleep apnea diagnosed?
Getting a sleep apnea diagnosis involves a sleep study, officially called a polysomnography. During this test, you sleep in a lab or hospital while hooked up to equipment that monitors your heart, lung and brain activity, arm and leg movements, breathing patterns and blood oxygen levels. It's also possible to do a sleep study at home in some areas, so you can ask your HCP whether this is an option for you.
If you have insurance, you may want to check whether your plan covers a sleep study and other services related to sleep apnea. If you're uninsured, some organizations offer assistance.
Who is at risk for sleep apnea?
Sleep apnea can affect anyone, but certain factors increase your risk. They include:
- Obesity
Excess weight around your airway can obstruct breathing. About 70% of adults with obstructive sleep apnea have obesity. The higher a person's BMI, the more likely they are to have the disorder.
- Advanced age
Sleep apnea is more common in people over age 50.
- Family history
Sleep apnea is partially caused by genetics in combination with environmental factors.
- Alcohol and sedatives
Both alcohol and sedatives like opioids relax the muscles in your throat, potentially obstructing your airway.
- Smoking
Smoking can cause inflammation and fluid accumulation in the airway and has been strongly linked to obstructive sleep apnea.
- Polycystic ovary syndrome (PCOS)
Women with PCOS are more likely to have sleep issues, including obstructive sleep apnea.
Patel says that, although sleep apnea affects more men than women, a woman's risk increases as she gets older. "Men seem to have this diagnosis in early years but women 'catch up' in post-menopausal years," she said. "Among older adults, women's prevalence of sleep apnea approaches that of men's." Patel adds that hormonal shifts contribute to the higher occurrence of sleep apnea in post-menopausal women.
Mistaking sleep apnea for menopause
As a woman's risk of sleep apnea increases around menopause, so does the likelihood she'll mistake sleep apnea symptoms for menopausal ones. Women and their HCPs may assume signs like frequent waking are related to menopause without considering other causes.
"There's sound research that the symptoms of sleep apnea are frequently misinterpreted or underappreciated, not just by patients but also providers," said Dr. Kristen Zarfos, a breast surgeon, women's health advocate and WHAC member.
"When a woman is awakened at night drenched in sweat and she happens to be the age that menopause could be occurring for her, it seems the symptoms are either discounted, or they're just assumed to be menopause," Zarfos said.
Patel agrees. "Women may often go undiagnosed or be misdiagnosed, especially if they don't present with classic sleep apnea symptoms," she said.
What happens if sleep apnea goes untreated?
The lapses in breathing that happen with sleep apnea keep your body from getting enough oxygen, leading not just to poor sleep but to potentially serious health consequences such as high blood pressure, diabetes, heart disease and stroke. Sleep apnea is also associated with both cognitive decline and dementia.
"Unfortunately, I don't think people know all the consequences of untreated sleep apnea," Patel said. "They don't realize how serious it can be."
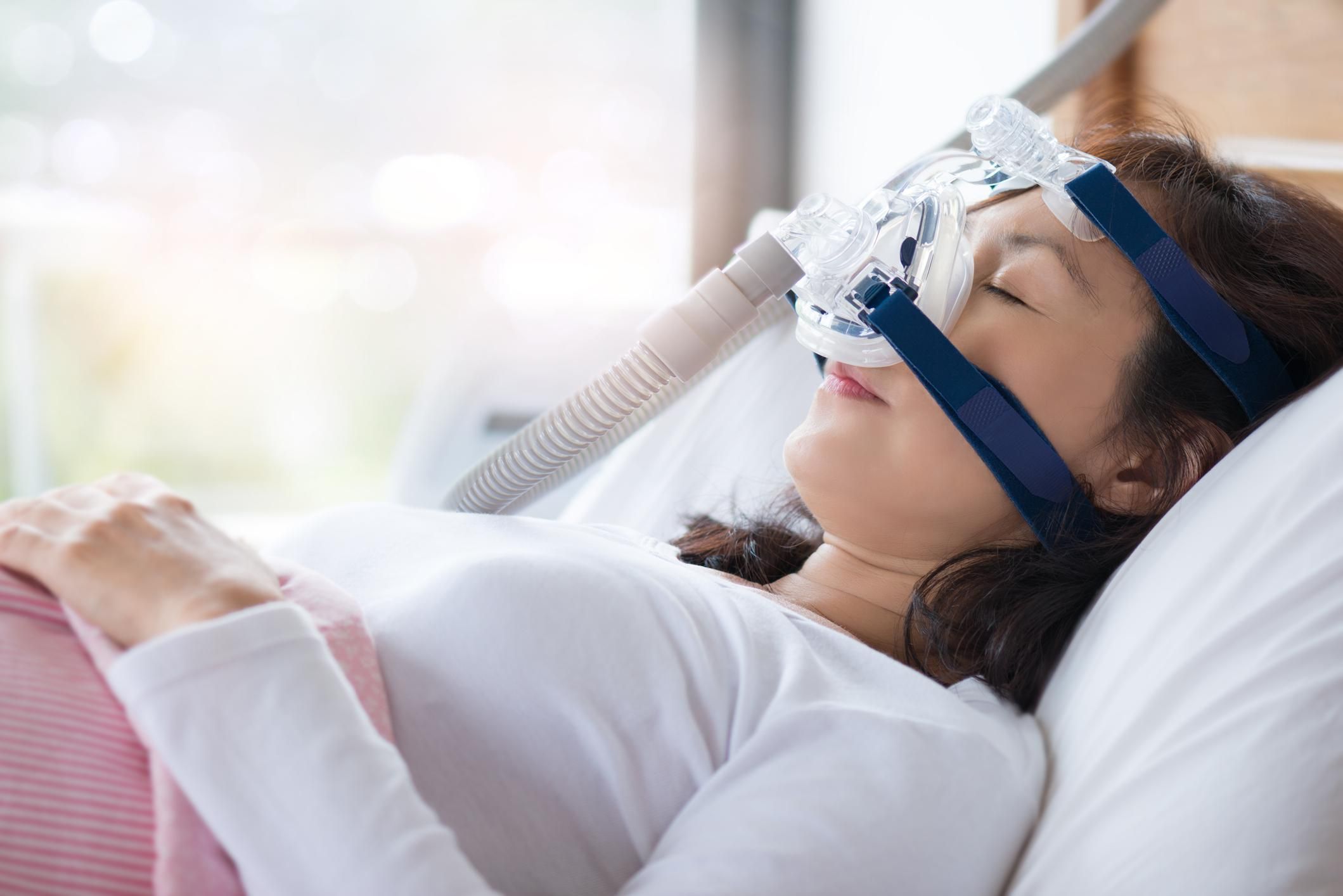
Treating sleep apnea
Sleep apnea is generally treated with a continuous positive airway pressure (CPAP) machine, which pushes a steady stream of air through a mask that you wear while sleeping, and oral appliances.
Both Patel and Zarfos note that a stigma exists around sleep apnea treatment that might prevent people from bringing their sleep problems up with an HCP. "I wish more women would discuss their sleep troubles with physicians and stay open to being evaluated," Patel said. She adds that advances in technology have led to new and more comfortable CPAP mask options.
According to Zarfos, it's really important for women to discuss their sleep issues with their HCP. The benefits of sleep apnea treatment far outweigh perceived unpleasantness. "Not only can it potentially save your life, but it can make the quality of your life so much better," she said. "It's well worth any mild discomfort or inconvenience."
Six years after her sleep apnea diagnosis, Christian is sleeping better than ever. She admits her CPAP machine took some getting used to, but now she can't imagine life without it.
"I'm thrilled I have it," Christian said. "I really feel like I'm healthier because of it."
- Not Just a Man's Disease—Women Get Sleep Apnea, Too! ›
- Sleep Apnea Is More Common Than You Think — and More Serious ›
- Menopause and Sleep: What's the Connection? - HealthyWomen ›
- Things You Should Know If You Wear a CPAP Mask - HealthyWomen ›
- Do You Suffer from Sleep Issues? These Resources Can Help ... ›
- Sleep Disorders - HealthyWomen ›
- Why Is My Sleep Apnea Making Me So Tired During the Day ... ›
- 5 Things That Sabotage Your Sleep - HealthyWomen ›