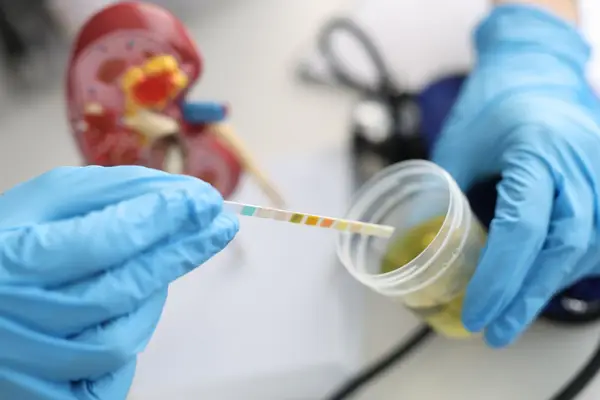
It sits near the pubic bone. When it's empty, it's about the size and shape of a pear. This sac, lined with layers of muscle tissue, stretches to hold urine, up to about 600 mL.
In the perfect world, your bladder would operate perfectly, filling and emptying without much fanfare.
But that's not always the case. There are numerous conditions that crop up, and some can make life complicated or difficult, not to mention embarrassing to talk about.
Cystitis
A urinary tract infection that can be painful, it's most commonly caused by bacteria. The bacteria are always present in the vaginal area, but cause problems when they enter the urinary tract. Cystitis can result from sexual intercourse, but you need not have sex to contract cystitis. It can also be caused by chemicals in personal care products, chemotherapy drugs or damage to your bladder from a catheter. Cystitis can be successfully treated with antibiotics or a vaginal cream.
Signs of Cystitis
- Trouble urinating or the urge to urinate more often than usual
- Pain or stinging when you urinate
- Achy and tired (sometimes with a fever)
- Pressure or pain in the lower abdomen
- Dark, cloudy or strong-smelling urine
How to avoid it
- Urinate after sex
- Avoid perfumed soaps, powders and bubble baths
- Don't ignore the need to urinate
- Wipe from front to back after you use the toilet
Interstitial Cystitis
This is a chronic form of cystitis, also known as painful bladder syndrome. The condition causes bladder pain and pressure and sometimes pelvic pain as well. Symptoms vary over time, ranging from mild to severe. Although it may feel as if you have a urinary tract infection, there is no infection. The exact cause is unknown, but some theories exist. One is that interstitial cystitis is caused by a defect in the bladder's protective lining (epithelium), through which toxic substances can enter and irritate the bladder wall. Other possibilities are an autoimmune condition, genetics, allergy or infection.
Understandably, the condition can really interfere with the quality of your life. Various treatments are available, including oral medications, physical therapy, nerve stimulation, stretching of the bladder, medications inserted directly into the bladder and surgery. Two complementary and alternative therapies, acupuncture and guided imagery, are showing promise in the treatment of interstitial cystitis.
Signs of Interstitial Cystitis
- Painful intercourse
- Pain between the vagina and anus
- Persistent and urgent need to urinate
- Frequent urination (but only small amounts are expelled) of up to 60 times a day
If you leak urine involuntarily you suffer from incontinence. Millions of Americans—mostly women—suffer from it. And it doesn't always take much to set it off. You may find that you leak when you cough, sneeze, exercise or lift something heavy. For some, even laughing can do it.
Stress incontinence happens because pelvic floor muscles and tissues can become weak from pregnancy and childbirth. Being overweight or obese or taking certain medications can also be a factor, as can menopause or hysterectomy.
With urge incontinence, you have a sudden and intense need to urinate, but can't make it to the bathroom in time. And that need is frequent, occurring many times throughout the night. Urge incontinence can result from an infection or something more serious like a neurologic disorder or condition like diabetes, stroke, Parkinson's disease or multiple sclerosis.
Overflow incontinence is when your bladder doesn't empty completely. As a result, you experience regular or continual "dribbling" of urine.
Some women will have mixed incontinence, when stress and urgency incontinence occur together. According to research, between 25 percent and 45 percent of women have some degree of urinary incontinence.
There are s a variety of treatments, both nonsurgical and surgical, including pelvic floor (Kegel) exercises, bladder retraining drills timed voiding, protective garments and pads, acupuncture, weight loss, pessaries, bladder slings, nerve stimulation, vaginal cream estrogen and various oral medications. Studies have shown that Botox can also help with symptoms of incontinence.
How to avoid it
- Practice pelvic floor exercises (Kegels)
- Use biofeedback to help train you to recognize when your bladder muscles squeeze
- Stay away from things that irritate the bladder like caffeine, alcohol and acidic foods
- Maintain a healthy weight
Recently cleared by the U.S. Food and Drug Administration and coming available in December 2017 will be a noninvasive electromagnetic energy treatment. Available in doctors' offices, BTL Emsella is a chair-like device that helps stimulate and strengthen pelvic floor muscles with high-intensity focused electromagnetic energy that causes the pelvic floor muscles to contract, restoring neuromuscular control.
Just one session (about 30 minutes) is equivalent to doing 11,000 Kegels. A series of six, twice-weekly treatments are suggested for optimal results, with a maintenance session needed once a year. The price varies by physician, averaging $300 to $500 per treatment. The treatment is not currently covered by insurance.