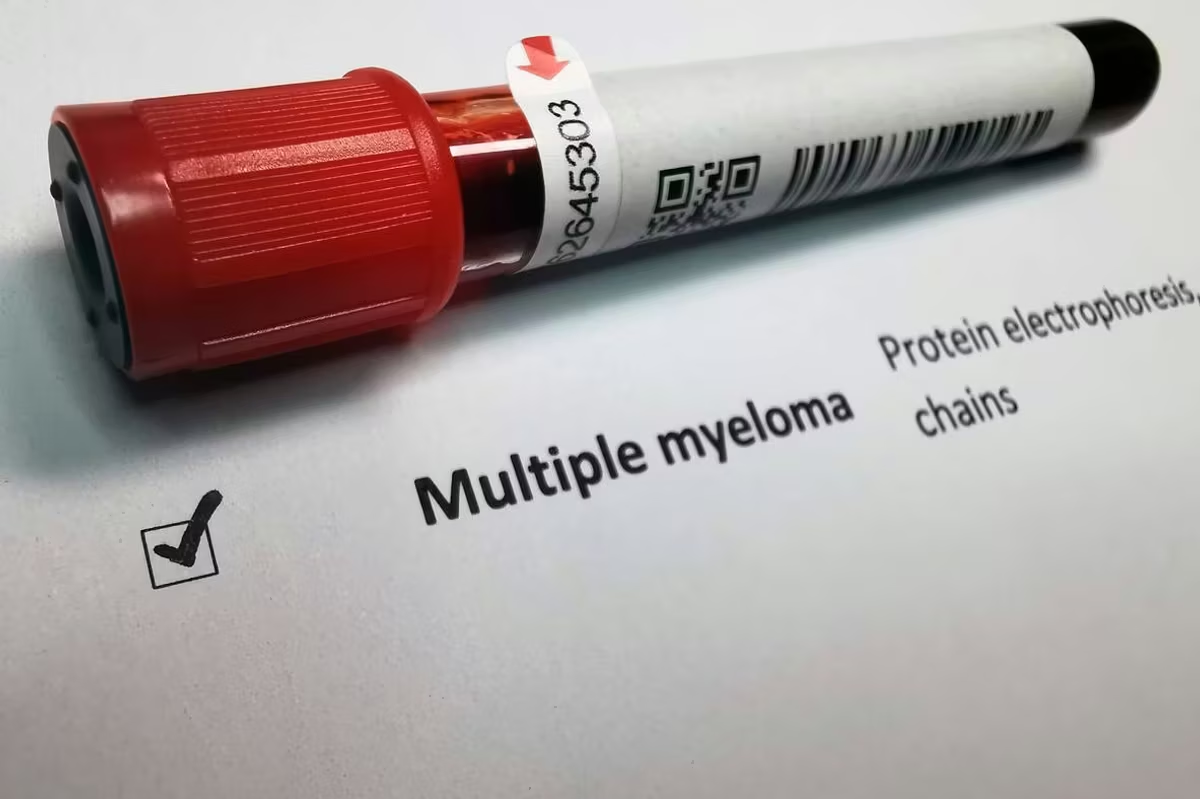
March is Multiple Myeloma Awareness Month.
Multiple myeloma, also sometimes just called myeloma, is a blood cancer that affects thousands of people each year.
Here’s what you need to know about multiple myeloma — what it is, how it’s managed and steps you can take to get an early diagnosis, so treatment can begin as soon as possible.
What is multiple myeloma?
Multiple myeloma is a rare type of cancer that starts in plasma cells, which are a type of white blood cell. Plasma cells make antibodies that help you fight infections. They’re found in the bone marrow, which is the soft inside part of bones where your body makes blood cells.
How does multiple myeloma develop?
When plasma cells become abnormal, or cancerous, they multiply quickly and crowd out healthy plasma cells. Instead of performing their normal job of making antibodies to protect you against germs, the cancerous cells start making an abnormal antibody called monoclonal protein (M protein).
What are the risk factors for multiple myeloma?
There isn’t a clear reason why some people get multiple myeloma and others don’t. But certain factors can increase the risk of developing the condition.
Some of the risk factors for multiple myeloma include:
- Being over age 65
- Being Black
- A family history of multiple myeloma
- Living with overweight or obesity
- Having another plasma cell disease
- Exposure to radiation and some chemicals, such as pesticides or fertilizers
What are the symptoms of multiple myeloma?
Multiple myeloma may not cause any symptoms. But when it does, you might experience symptoms such as:
- Pain in your bones, especially in the back and ribs
- Broken bones or fractures
- Feeling weak or fatigued
- Weight loss you can’t explain
- Frequent infections and fevers
- Feeling thirsty all the time
- Needing to pee often
What health complications can multiple myeloma cause?
Multiple myeloma can cause other health conditions, including:
- Frequent infections
- Bone problems, including pain, fractures and thinning
- Kidney problems, including kidney failure, which is when your kidneys can’t properly remove waste from the body
- Anemia, or low red blood cell count
- High blood calcium levels, known as hypercalcemia
How is multiple myeloma diagnosed?
If your healthcare provider (HCP) thinks you have multiple myeloma, or if you are having symptoms, you will have testing done to confirm the diagnosis. If you have no symptoms, multiple myeloma may be found during testing for another health condition.
- Blood and urine tests can detect M proteins. A blood test can also discover other proteins made by myeloma cells, such as beta-2-microglobulin. Other blood tests can include complete blood count tests to check your kidney function, and calcium and uric acid levels.
- Imaging tests like X-rays, CT scans, MRI scans and positron emission tomography (PET) scans may be used to look for any bone problems.
- A bone marrow biopsy is a test where your HCP inserts a needle into the bone marrow space — usually from the hip — to collect tissue for testing. This tissue will be studied under a microscope to look for myeloma cells.
Your HCP may also use the CRAB criteria to diagnose myeloma. CRAB stands for:
- High Calcium levels
- Renal (kidney) problems
- Anemia
- Bone damage
If your tests show M proteins in your blood without any other symptoms, you may be diagnosed with a condition that’s a precursor to multiple myeloma.
The two precursors are early-stage myeloma and include:
- Monoclonal gammopathy of undetermined significance (MGUS): Considered noncancerous, or benign, and doesn’t require treatment. About 1% of people with MGUS will eventually have active myeloma.
- Smoldering multiple myeloma (SMM): Considered precancerous, and if treatment is needed, it will likely take place in a clinical trial. About 1 out of 10 people with SMM will get myeloma.
If active myeloma is found, it will be staged from 1 to 3. Stage 1 myeloma grows slowly, while stage 3 is faster-growing and more aggressive. Determining the stage helps your HCP figure out the best treatment plan for you.
What are the treatment options for multiple myeloma?
Treatments for multiple myeloma can include:
- Targeted chemotherapy — specifically attacks cancer cells
- Immunotherapy — uses your body’s own immune system to attack cancer cells
- Stem cell transplant — replaces cancerous bone marrow with healthy bone marrow
- CAR-T cell therapy — a type of immunotherapy that uses T cells from your blood to fight the cancer
- Corticosteroids — target and destroy myeloma cells
- Radiation — quickly shrinks a mass of myeloma cells
There is no cure for multiple myeloma, but it can be managed with treatment. Multiple myeloma has a five-year survival rate of about 62%. This means about 6 out 10 people with myeloma are still alive five years after they were initially diagnosed.
Clinical trials are a way to get involved in new myeloma treatments. Talk to your HCP about your options, and check out the National Cancer Institute’s list of active clinical trials for multiple myeloma.
This educational resource was created with support by an educational grant from Johnson & Johnson.