Vision loss is scary, especially for people like me whose livelihoods depend on good vision. I recently had successful emergency laser surgery to prevent a retinal tear and possible retinal detachment, and I'm sharing my experience to help others recognize the symptoms that could save your vision.
Saturday night I started seeing flashes of light that looked like lightning. They popped up on the right side of my field of vision and sort of leaped at a right angle across the top of my sight. Each flash was quick, and the time between flashes varied.
I thought it might be a migraine aura, but I've had those in the past, and this seemed different. My auras last precisely 20 to 23 minutes and appear like a tunnel of light. These looked different and continued well beyond 20 minutes.
Because I was riding in the backseat of a car with my younger daughter driving on very dark, unfamiliar, winding rural roads in the rain, I didn't want to say anything that might add to anyone's stress. So I alternately closed my eyes to avoid seeing the light and searched on my phone for what could be causing the flashes.
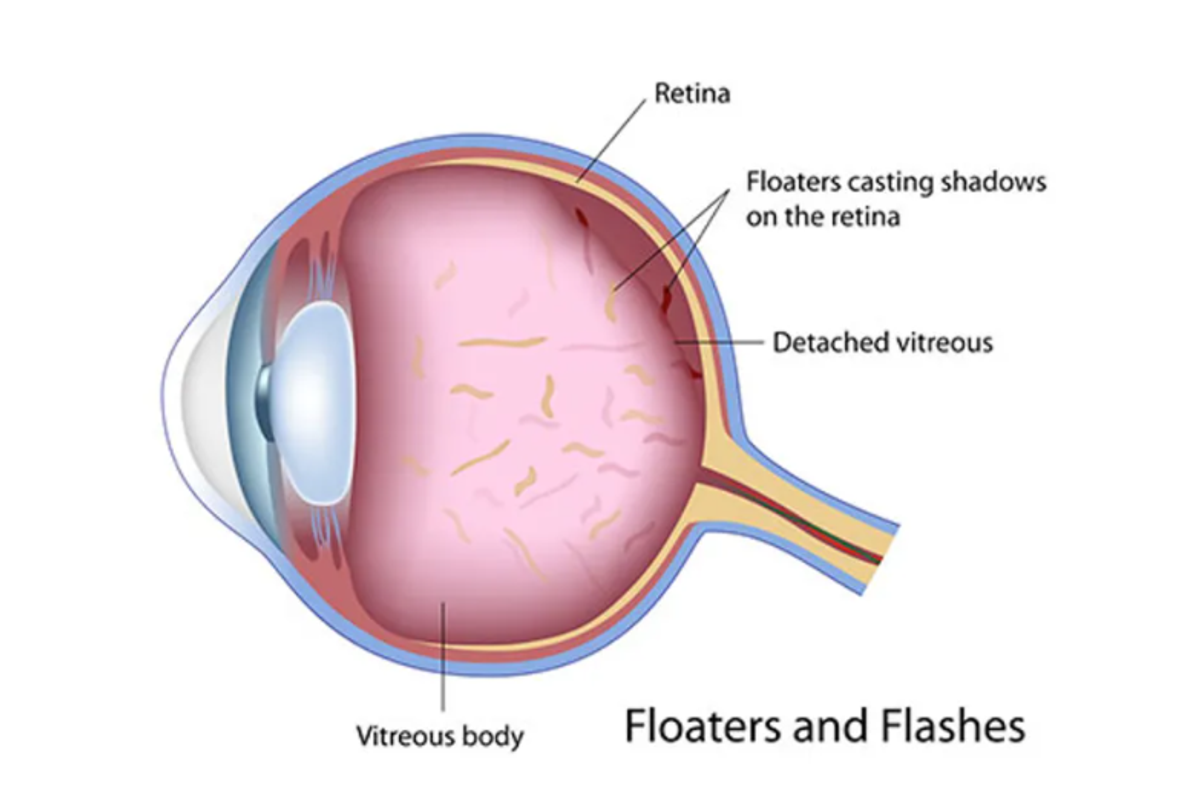
My online searches, using reliable sites like the Mayo Clinic and Cleveland Clinic, revealed that light flashes are a symptom of a retinal tear or detachment. A retinal detachment can occur when the vitreous, a gel-like fluid inside the eye, leaks through a retinal hole or tear and collects beneath the retina at the back of the eye. This causes the retina to pull away from the blood vessels that provide it with oxygen and nourishment, resulting in vision loss. Retinal detachment is an emergency because the longer it goes untreated, the greater your risk of vision loss.
The vitreous normally shrinks and detaches as we age and doesn't cause problems, other than pesky floaters (specks of debris that seem to float through your vision). But, if the vitreous doesn't detach easily and instead tugs on the retina, it can cause tears. That's why it's important to know what to look for to avoid retinal detachment.
Symptoms of retinal tears or detachment include:
- Light flashes
- Sudden appearance of many floaters
- A shadow or curtain over part of your visual field (usually this comes as detachment progresses; thank goodness mine didn't go that far)
So, when we got home around 7 o'clock Saturday night, I told my family what was going on. I wasn't certain from the websites how urgent the situation was—whether I should go to the ER, call a doctor or take it easy and wait until Monday.
My two daughters quickly decided that I should call a medical professional for clarification, especially since the next day was Sunday and I wouldn't be able to see my eye doctor until Monday at the earliest. My husband told me it wouldn't do any good to go to the emergency room—advice my eye doctor later confirmed, because the eyes need to be dilated by an ophthalmologist to be examined.
I found my ophthalmologists' phone number online and discovered that they have an after-hours emergency number, which I dialed. I was put directly through to the on-call doctor. He listened to my symptoms and asked a few questions, such as how long I'd been seeing the flashes (2.5 hours), my age (60) and whether I was nearsighted (yes, slightly) or had diabetes (no).
Risk factors for retinal detachment include:
- Aging (it is more common in people over age 40)
- Previous retinal detachment or eye surgery
- Family history
- Extreme nearsightedness
- Previous severe eye injury or trauma
- Previous eye disease or disorder
The doctor asked if I could meet him at the office at 9 p.m. (seriously, 9 o'clock on a Saturday night!). I felt a little relieved and a little scared—relieved that someone was available to look at my eyes at night on a weekend and scared that either something would be wrong with my vision or that it wouldn't and this would all be a very expensive false alarm.
My husband and I and the doctor and an assistant arrived at about 8:45, and he took me in to dilate and examine my eyes. After a first look, he said he didn't see anything obvious, but there was one area he wanted to take a closer look at. So, he applied more numbing drops and stuck a magnifying lens on my right eyeball, held in place by what he scientifically described as goop.
After closer examination, he said the vitreous fluid in my right eye was trying to detach but was not separating easily and was tugging on the back of my retina, which showed signs of compromise and weak spots—on the verge of tearing.
He said I had two options: I could do nothing (a very, very bad option, he said) or I could have laser surgery to repair it—immediately. Because I very much value my vision, I opted for laser surgery.
Undergoing laser surgery
He got everything ready, put a powerful lens back on my eyeball and told me to keep my forehead and chin pressed against the stabilizing bars and keep my head as still as possible. He warned me that the laser might give a sensation of heat or pressure, but no real pain.
Then he began zapping my eyeball with a laser. The laser makes tiny burns around the tears or weak spots to create scarring that "welds" the retina to the underlying tissue. I could feel both warmth and pressure from the laser, but the worst sensation for me was the feeling of bright light in my eye. I felt like I'd closed my eye to block out the light, but, in reality, the lens kept the eye open. I'm not sure how many times he zapped my retina or how long it took, but the whole procedure was relatively quick and painless.
He told me that no postsurgical care or recuperation was required because there was no cutting, no pain, no risk of infection. (Mayo Clinic says you may be advised to refrain from vigorous activities for a couple of weeks to allow the bonds to strengthen, but I was not told to take it easy.) My doctor said I might continue to see occasional flashes for a while as the vitreous fluid continued to separate (which I did), but there should be no more danger of retinal tears or detachment.
Almost exactly an hour after I entered the office on a Saturday night, I was on my way home with my vision problem corrected and my vision intact.
What I've learned through this is that early diagnosis is critical to preventing retinal detachment and possible permanent vision loss. It's important to get your eyes checked annually, especially as you age or if you have other risk factors for retinal detachment. Talk to your eye care professional if you aren't sure about your risk.
And if you notice any symptoms of a possible retinal tear or detachment, call your eye doctor immediately. The procedures to repair retinal detachment are more complex than what I had, and success is not guaranteed.
I am grateful to my job at HealthyWomen for making me more aware of taking care of my health and paying attention to symptoms. I'm grateful to my daughters for encouraging me to seek immediate care. I'm grateful to my husband for taking me to the doctor's and keeping me calm. And I'm especially grateful that the on-call ophthalmologist was willing to record the rest of the football playoffs he was watching and come in on a Saturday night to take care of my vision.