April is Parkinson’s Disease Awareness Month.
On a recent episode of the popular Apple TV show Shrinking, actor Michael J. Fox made a cameo as a real-life representation of someone living with Parkinson’s disease.
“I fall three times a day,” he said. “I’m thinking of becoming a stunt man.”
Balance issues and uncontrollable body tremors are common symptoms of Parkinson’s disease. The progressive brain disorder happens when there’s damage to dopamine-producing neurons in the part of the brain that controls movement — hence the involuntary muscle contractions. The disease can also cause non-motor symptoms including sleep disorders and constipation.
The cause of Parkinson’s disease is unknown, but a growing body of research suggests the gut microbiome might have something to do with it.
What is the gut microbiome?
Your gut microbiome is a wild world of trillions of microorganisms including bacteria, viruses and fungi that reside in your digestive system.
The complex ecosystem of microbes plays a big part in your health and overall well-being. “The gut microbiome has many diverse functions such as the production of short-chain fatty acids, some vitamins and neurotransmitters, influencing immune system development and regulation, and helping maintain intestinal barrier integrity,” said Kaylyn Koons, MS, RD, LD, a clinical dietitian at Norman Fixel Institute for Neurological Diseases.
Everyone’s gut microbiome is unique with microorganisms that are shaped by genetics, early-life experiences (birth method and formula vs. breastfeeding), lifestyle habits and environment among other factors.
The gut microbiome and Parkinson’s disease
People with Parkinson’s disease often have distinct changes in their gut microbiome compared to people who don’t have Parkinson’s.
Research shows people with Parkinson’s have reduced overall microbiome diversity, which comes from an imbalance in the microbiome, known as dysbiosis. This means the gut microbiome has an increased amount of bacteria that cause inflammation and a reduced amount of beneficial microbes compared to healthy gut microbiomes. And dysbiosis increases the risk for chronic diseases like Parkinson’s.
Koons said people with Parkinson’s disease also show changes within the metabolites (molecules needed for basic survival) produced in the microbiome. These changes include reduced production of short-chain fatty acids and increased production of the metabolite trimethylamine N-oxide — a potential biomarker of Parkinson’s disease.
This is significant because reduced levels of short-chain fatty acids can lead to the breakdown of the intestinal barrier — also known as a leaky gut — triggering inflammation in the brain and misfolding of a protein called alpha-synuclein, which is a key hallmark of Parkinson's disease.
The brain-gut axis and Parkinson’s disease
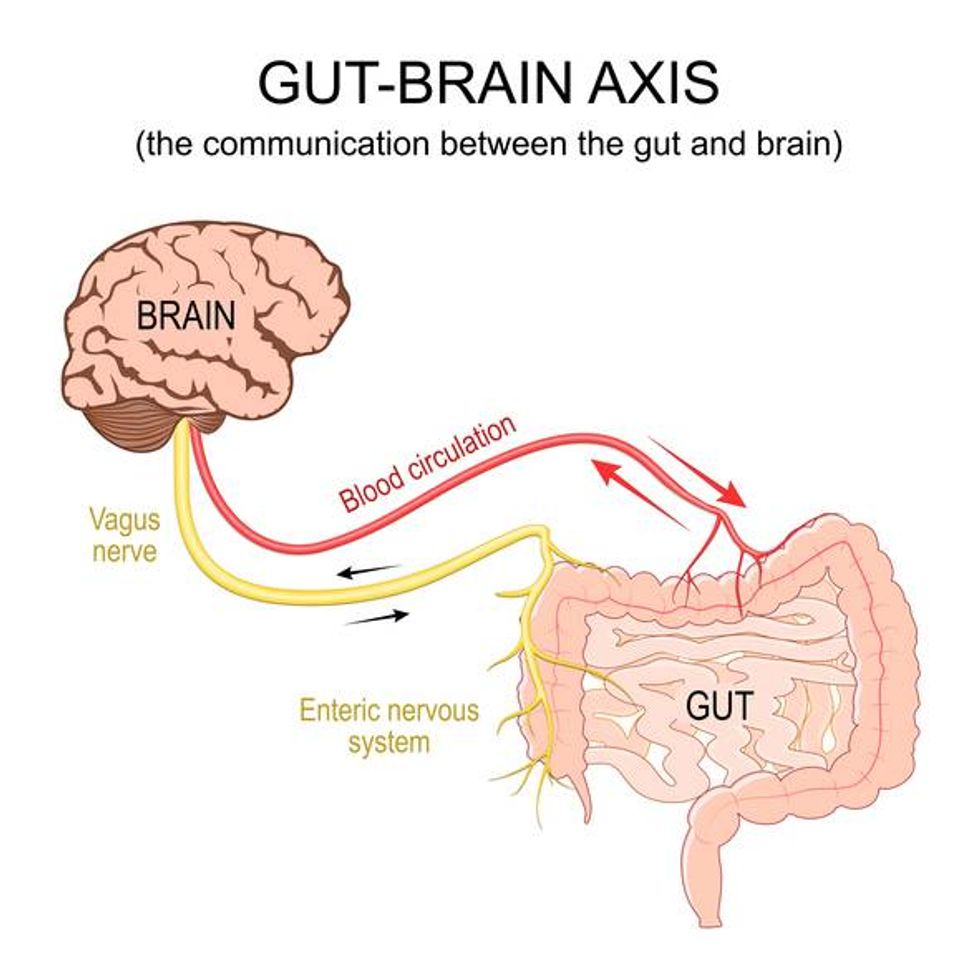
iStock.com/ttsz
Although Parkinson’s is a brain disorder, there’s been an increased interest in the idea that the disease develops in the gut.
A 2019 study found that the misfolded proteins that damage and kill neurons in the brain originate in the gut and travel to the brain via the vagus nerve.
When the abnormal proteins accumulate in the gut and the enteric nervous system, they cause symptoms like constipation, which is very common in people with Parkinson’s disease.
“Non-motor symptoms of Parkinson’s disease affect multiple organ systems, including the gastrointestinal system and have been found to predate motor symptoms for years — even decades,” Koons said.
Research also shows that common gastrointestinal (GI) conditions such as gastroesophageal reflux disease and H. pylori infections may be early risk factors to consider. One recent study found damage to the lining of the upper digestive tract — erosions, esophagitis, ulcers or peptic injury — was associated with a 76% greater risk of developing Parkinson’s.
Although research is ongoing regarding the exact role gut health plays in the development or progression of Parkinson’s, the gut-first hypothesis could mean new ways of finding and treating the disease.
How to support your gut microbiome if you have Parkinson’s disease
Many people with Parkinson’s disease experience digestive problems that affect the entire system, from difficulty swallowing to delayed stomach emptying. In fact, nearly 4 out of 5 people with Parkinson’s experience GI problems, and women can have more severe GI symptoms than men.
“Women experience significantly higher levels of fullness after eating, inability to finish a regular size meal and pain in the upper abdomen,” Koons said.
For people living with Parkinson’s disease, a high-fiber eating plan can help keep GI symptoms at bay and balance the gut microbiome. When gut bacteria break down fiber, the process produces short-chain fatty acids, which can boost the gut’s mucus barrier to fight inflammation and protect the brain.
Incorporating fermented food or foods that contain live cultures such as yogurt can help balance the good bacteria in the gut and keep digestion on track.
Koons recommends the Mediterranean diet for her patients with Parkinson’s. “The Mediterranean diet is associated with increased beneficial bacteria such as Faecalibacterium prausnitzii and Bifidobacterium bifidum and greater production of short-chain fatty acids,” she said.
Although there’s no cure for Parkinson’s disease, managing GI problems can help with non-motor symptoms and improve overall well-being. If you’re living with Parkinson’s disease, talk to your healthcare provider about what you can do to keep your gut as healthy as possible.