
Learn about our editorial policies
Medically Reviewed
THURSDAY, Dec. 18, 2014 (HealthDay News) -- Few people know how to properly use the medical devices that contain lifesaving medications for severe allergic reactions and asthma attacks, a new study shows.
Just 16 percent knew the correct way to use an epinephrine injector for someone with a life-threatening allergy. And only 7 percent knew how to use an asthma inhaler as directed.
"This isn't a new concern. We always worry about our patients, especially those with food allergies," said one of the study's authors, Dr. Aasia Ghazi, from the Allergy and Asthma Specialists of Dallas.
"We had a patient call in the middle of a reaction, and she didn't remember how to use the epinephrine injector. That's why we looked to see what's going on, and what are the barriers that keep patients from using these devices properly?" Ghazi explained.
The study was published online Dec. 18 in the Annals of Allergy, Asthma and Immunology.
A life-threatening allergic reaction is known as anaphylaxis. The incidence of anaphylaxis is rising, according to background information in the study. A shot of epinephrine -- a stimulating hormone -- into a muscle can stop anaphylaxis, according to the study authors.
"A life can be saved with an epinephrine injection. It's a big deal," said Ghazi.
Asthma inhalers can be used to deliver medicine to stop an asthma attack, or they can deliver preventive medications that help stop asthma attacks from occurring. They can be used alone or along with an additional device called a spacer. Spacers are chambers that temporarily hold the medication, which can be especially helpful when giving medication to children, according to the American Lung Association.
Misuse of asthma inhalers or spacers can lead to too little medicine being used. That means symptoms might not be treated properly. It can also lead to overuse of medication, according to background information in the study.
Ghazi and her colleagues recruited 102 patients prescribed epinephrine and 44 prescribed asthma inhalers or spacers for the study. Eleven percent of those prescribed epinephrine had used the device before. Eighty percent of those with asthma reported having used an inhaler -- also called a metered-dose inhaler, or MDI -- or a spacer before, the researchers said.
The study volunteers demonstrated how to use a device to the researchers.
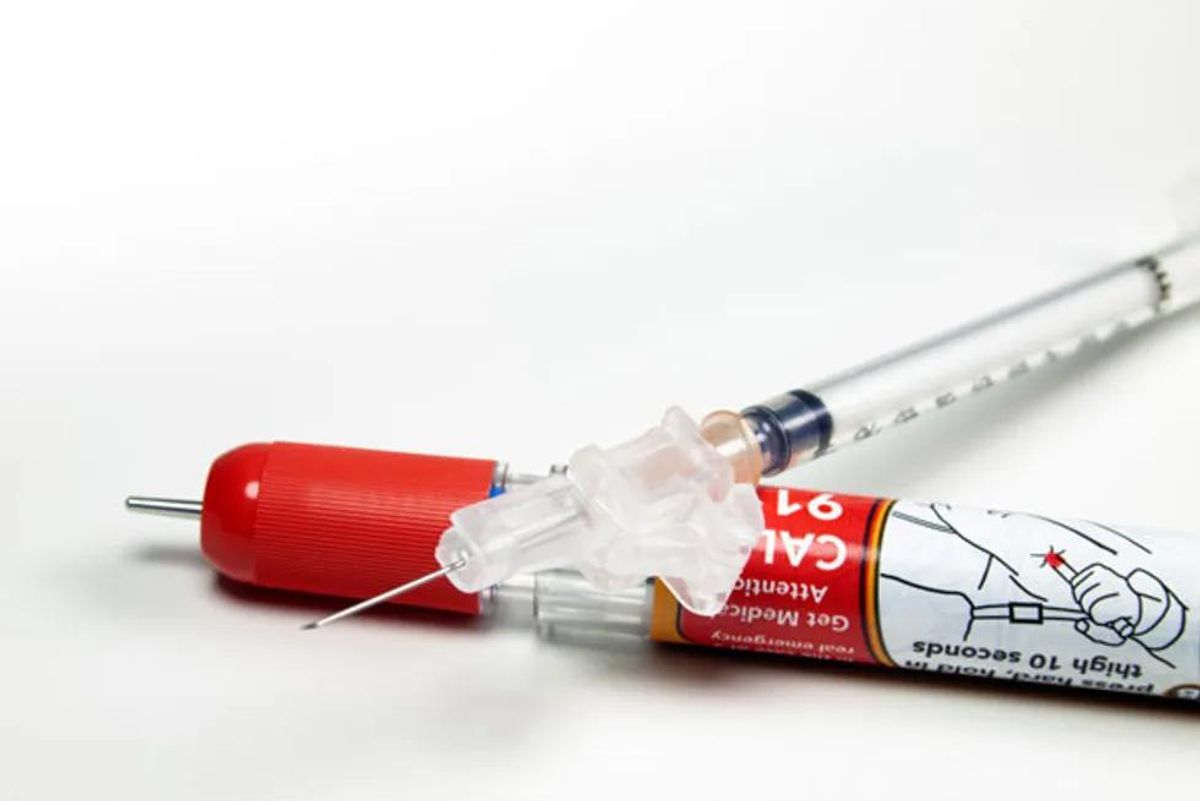
Of the 84 percent who misused the epinephrine, more than half missed three or more steps involved in the correct use of the device. The most common error was not leaving the shot in for 10 seconds.
"We instruct patients to leave the unit in place for 10 seconds to make sure 100 percent of the medication is injected," Ghazi said.
Of the 93 percent who misused asthma inhalers or spacers, 63 percent missed three or more steps. The most common mistake was not exhaling before depressing the canister to inhale the medication, according to the study.
Time appeared to be a significant factor in patients' memories. For those prescribed epinephrine injectors within a year, 10 percent had perfect use. If they had the device for one to five years, just 5 percent had perfect use. If someone had been given the device five years prior, perfect use dropped to just 1 percent, the study found.
"This study really drives home the need to reinforce the use of these devices every time a patient comes in," said Dr. Jennifer Appleyard, chief of allergy and immunology at St. John Providence Health System in Detroit. "And, it's not enough to just give instructions. People need to show me how they use the device," she added.
Appleyard, who was not involved with the study, said that epinephrine injectors come in kits that have training devices. She also suggested practicing with expired devices by injecting a piece of fruit, such as an orange. "It's important to feel comfortable with the injector. Everyone needs to practice," Appleyard said.
Some devices have instructions written on them, and others will talk you through the steps, according to Ghazi.
Both experts said if your doctor hasn't shown you how to use your medical devices, you need to speak up. "Talk to your caregiver, and make sure you're getting instructions whenever you visit. Make sure you're getting it right, and clarify any doubts you have," Ghazi said.
SOURCES: Aasia Ghazi, M.D., Allergy and Asthma Specialists of Dallas, and adjunct assistant professor, University of Texas Medical Branch, Galveston, Texas; Jennifer Appleyard, chief of allergy and immunology, St. John Providence Health System, Detroit; Dec. 18, 2014, Annals of Allergy, Asthma and Immunology, online
Copyright © 2014 HealthDay. All rights reserved.
You might be interested in





